The Nuevo health plan's capital structure consists of 30% debt and 70% equity. Nuevo's average after-tax cost of debt is 6% and its cost of equity is 12%. The following statement(s) can correctly be made about Nuevo's weighted average cost of capital (WACC):
Many clinicians are concerned about the development of practice guidelines that seek to define appropriate healthcare services that should be provided to a patient who has been diagnosed with a specific condition. To avoid the risk associated with using such guidelines, health plans should advise clinicians that the existence of such a guideline:
1. Establishes standards of care to be routinely utilized with all patients presenting a specific condition
2. Preempts a physician’s judgment when assessing the specific factors related to a patient’s condition
The following information was presented on one of the financial statements prepared by the Rouge health plan as of December 31, 1998:
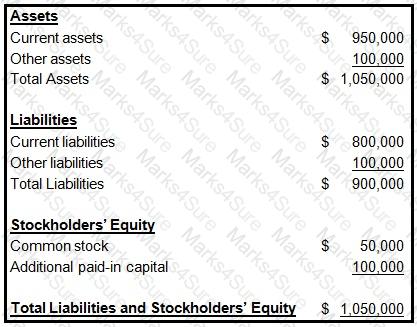
When calculating its cash-to-claims payable ratio, Rouge would correctly divide its:
The following examples describe situations that expose an individual or a health plan to either pure risk or speculative risk:
Example 1 — A health plan invested in 1,000 shares of stock issued by a technology company.
Example 2 — An individual could contract a terminal illness.
Example 3 — A health plan purchased a new information system.
Example 4 — A health plan could be held liable for the negligent acts of an employee.
The examples that describe pure risk are
Mandated benefit laws are state or federal laws that require health plans to arrange for the financing and delivery of particular benefits. Ways that mandated benefits have the potential to influence health plans include:
1. Causing a lower degree of uniformity among health plans of competing health plans in a given market
2. Increasing the cost of the benefit plan to the extent that the plan must cover mandated benefits that would not have been included in the plan in the absence of the law or regulation that mandates the benefits
The Wallaby Health Plan purchased an asset two years ago for $50,000. At the time of purchase, the asset had an appraised value of $52,000. The asset carries a value on Wallaby’s general ledger of $47,000, and its current market value is $80,000. According to the cost concept, Wallaby would report on its financial statements a value for this asset equal to:
Correct statements about the financial risks associated with benefits that health plans provide to the Medicare and Medicaid markets include:
The process of converting the present value of a specified amount of money to its future value is known as
A health plan may experience negative working capital whenever healthcare expenses generated by plan members exceed the premium income the health plan receives.
Ways in which a health plan can manage the volatility in claims payments, and therefore reduce the risk of negative working capital, include:
1. Accurately estimating incurred but not reported (IBNR) claims
2. Using capitation contracts for provider reimbursement
A primary reason that a financial analyst would measure the Tapestry health plan's return on assets (ROA) is to determine the
The types of financial risks and costs to which a health plan is subject depends on whether the health plan provides services to the Medicare and/or Medicaid populations or to the commercial population. One distinction between providing services to the Medicare and Medicaid populations and to the commercial population is that Medicare and Medicaid enrollees typically:
The Titanium health plan's product has a unit price of $120 PMPM and a unit variable cost of $80 PMPM. Titanium has $100,000 in fixed costs per month. This information indicates that, for its product, Titanium's
The following information relates to the Hardcastle Health Plan for the month of June:
Incurred claims (paid and IBNR) equal $100,000
Earned premiums equal $120,000
Paid claims, excluding IBNR, equal $80,000
Total health plan expenses equal $300,000
This information indicates that Hardcastle’s medical loss ratio (MLR) for the month of June was approximately equal to:
Julio Benini is eligible to receive healthcare coverage through a health plan that is under contract to his employer. Mr. Benini is seeking coverage for the following individuals:
Elena Benini, his wife
Maria Benini, his 18-year-old unmarried daughter
Johann Benini, his 80-year-old father who relies on Julio for support and maintenance
The health plan most likely would consider that the definition of a dependent, for purposes of healthcare coverage, applies to:
In a comparison of small employer-employee groups to large employer-employee groups, it is correct to say that small employer-employee groups tend to:
In order to analyze costs for internal management purposes, the Banner health plan uses functional cost analysis. One characteristic of this method of cost analysis is that it
The provider contract that Dr. Timothy Meyer, a pediatrician, has with the Cardigan health plan states that Cardigan will compensate him under a capitation arrangement. However, the contract also includes a typical low enrollment guarantee provision. Statements that can correctly be made about this arrangement include that the low enrollment guarantee provision most likely:
The Atoll Health Plan must comply with a number of laws that directly affect the plan's contracts. One of these laws allows Atoll's plan members to receive medical services from certain specialists without first being referred to those specialists by a primary care provider (PCP). This law, which reduces the PCP's ability to manage utilization of these specialists, is known as _________.
The Newfeld Hospital has contracted with the Azalea Health Plan to provide inpatient services to Azalea's enrolled members. The contract calls for Azalea to provide specific stop-loss coverage to Newfeld once Newfeld's treatment costs reach $20,000 per case and for Newfeld to pay 20% of the next $50,000 of expenses for this case. After Newfeld's treatment costs on a case reach $70,000, Azalea reimburses the hospital for all subsequent treatment costs.
One true statement about this specific stop-loss coverage is that
The Lighthouse health plan operates in a state that allows the health plan to use an underwriting method of determining a group's premium in which underwriters treat several small groups as one large group for risk assessment purposes. This method, which helps Lighthouse more accurately estimate a small group's probable claims costs, is known as
Rasheed Azari, the risk manager for the Tower health plan, is attempting to work with providers in the organization in order to reduce the providers' exposure related to utilization review. Mr. Azari is considering advising the providers to take the following actions:
1-Allow Tower's utilization management decisions to override a physician's independent medical judgment
2-Support the development of a system that can quickly render a second opinion in case of disagreement surrounding clinical judgment
3-Inform a patient of any issues that are being disputed relative to a physician's recommended treatment plan and Tower's coverage decision
Of these possible actions, the ones that are likely to reduce physicians' exposures related to utilization review include actions
The Eagle health plan wants to limit the possibility that it will be held vicariously liable for the negligent acts of providers. Dr. Michael Chan is a member of an independent practice association (IPA) that has contracted with Eagle. One step that Eagle could take in order to limit its exposure under the theory of vicarious liability is to
The Caribou health plan is a for-profit organization. The financial statements that Caribou prepares include balance sheets, income statements, and cash flow statements. To prepare its cash flow statement, Caribou begins with the net income figure as reported on its income statement and then reconciles this amount to operating cash flows through a series of adjustments. Changes in Caribou's cash flow occur as a result of the health plan's operating activities, investing activities, and financing activities.
The main purpose of Caribou's balance sheet is to
An actuary for the Noble Health Plan observed that the plan's actual morbidity was lower than its assumed morbidity and that the plan's actual administrative expenses were higher than its assumed administrative expenses. In this situation, Noble's actual underwriting margin was
The following statements are about various reimbursement arrangements that health plans have with hospitals. Select the answer choice containing the correct statement.
The Health Maintenance Organization (HMO) Model Act, developed by the National Association of Insurance Commissioners (NAIC), represents one approach to developing solvency standards. One drawback to this type of solvency regulation is that it
The provider contract that Dr. Zachery Cogan, an internist, has with the Neptune Health Plan calls for Neptune to reimburse him under a typical PCP capitation arrangement. Dr. Cogan serves as the PCP for Evelyn Pfeiffer, a Neptune plan member. After hospitalizing Ms. Pfeiffer and ordering several expensive diagnostic tests to determine her condition, Dr. Cogan referred her to a specialist for further treatment. In this situation, the compensation that Dr. Cogan receives under the PCP capitation arrangement most likely includes Neptune's payment for
With regard to the financial statements prepared by health plans, it can correctly be stated that
This concept, which holds that a company should record the amounts associated with its business transactions in monetary terms, assumes that the value of money is stable over time. This concept provides objectivity and reliability, although its relevance may fluctuate.
From the following answer choices, choose the name of the accounting concept that matches the description.
Under the alternative funding method used by the Flair Company, Flair assumes financial responsibility for paying claims up to a specified level and deposits the funds necessary to pay these claims into a bank account that belongs to Flair. However, an insurer, which acts as an agent of Flair, makes the actual payment of claims from this account. When claims exceed the specified level, the insurer pays the balance from its own funds. No state premium tax is levied on the amounts that Flair deposits into this bank account.
From the following answer choices, choose the name of the alternative funding method described.
The reimbursement arrangement that Dr. Caroline Monroe has with the Exmoor Health Plan includes a typical withhold arrangement. One true statement about this withhold arrangement is that, for a given financial period,
The following statements are about risk management in health plans. Select the answer choice containing the correct response.
For this question, select the answer choice containing the terms that correctly complete blanks A and B in the paragraph below. The FASB mandates that accounting information must exhibit certain qualitative characteristics. One of these characteristics is ________A________, which means that a company's financial statements use the same accounting policies and procedures from one accounting period to the next, unless there is a sound reason for changing a policy or procedure. Another characteristic is _________B________, which requires a company to disclose in its financial statements all significant financial information about the company.
State A, which requires guaranteed issue of at least two mandated healthcare plans, has established a typical health coverage reinsurance program for small employer groups. One true statement about this reinsurance program is that it most likely
The Kayak Company self funds the health plan for its employees. This plan is an example of a type of self-funded plan known as a general asset plan.
Because Kayak's plan is a general asset plan, the funds that Kayak sets aside for the health plan are
Most organizations that obtain group healthcare coverage can be classified as one of three types of groups: employer-employee groups, multiple employer groups, and professional associations. One true statement about these types of groups is that
In the following paragraph, a sentence contains two pairs of words enclosed in parentheses. Determine which word in each pair correctly completes the statement. Then select the answer choice containing the two words that you have selected.
The Igloo health plan recognizes the receipt of its premium income during the accounting period in which the income is earned, regardless of when cash changes hands. However, Igloo recognizes its expenses when it earns the revenues related to those expenses, regardless of when it receives cash for the revenues earned. This information indicates that the (realization/capitalization) principle governs Igloo's revenue recognition, whereas the (matching/initial-recording) principle governs its expense recognition.
The methods of alternative funding for health coverage can be divided into the following general categories:
Category A—Those methods that primarily modify traditional fully insured group insurance contracts
Category B—Those methods that have either partial or total self funding
Typically, small employers are able to use some of the alternative funding methods in
Experience rating and manual rating are two rating methods that the Cheshire health plan uses to determine its premium rates. One difference between these two methods is that, under experience rating, Cheshire
The Jasmine Company, which self funds the health plan for its 200 employees, has established a 501(c)(9) trust as a means of addressing possible claims fluctuations under the health plan. This plan is not a part of a collective bargaining process. A potential disadvantage to Jasmine of using a 501(c)(9) trust is that
With regard to capitation arrangements for hospitals, it can correctly be Back to Top stated that
The following statements are about federal laws and regulations which affect health plans that offer products and services to the employer group market. Select the answer choice containing the correct statement.
The following statements are about pure risk and speculative risk—two kinds of risk that both businesses and individuals experience. Select the answer choice containing the correct statement.
A key factor that distinguishes the various types of health plans is the type and amount of risk that a health plan assumes with respect to the delivery and financing of healthcare benefits. An example of a type of health plan that typically assumes the financial risk of delivering and financing healthcare benefits is a
The following statements illustrate common forms of capitation:
1. The Antler Health Plan pays the Epsilon Group, an integrated delivery system (IDS), a capitated amount to provide substantially all of the inpatient and outpatient services that Antler offers. Under this arrangement, Epsilon accepts much of the risk that utilization rates will be higher than expected. Antler retains responsibility for the plan's marketing, enrollment, premium billing, actuarial, underwriting, and member services functions.
2. The Bengal Health Plan pays an independent physician association (IPA) a capitated amount to provide both primary and specialty care to Bengal's plan members. The payments cover all physician services and associated diagnostic tests and laboratory work. The physicians in the IPA determine as a group how the individual physicians will be paid for their services.
From the following answer choices, select the response that best indicates the form of capitation used by Antler and Bengal.
The Newfeld Hospital has contracted with the Azalea Health Plan to provide inpatient services to Azalea's enrolled members. The contract calls for Azalea to provide specific stop-loss coverage to Newfeld once Newfeld's treatment costs reach $20,000 per case and for Newfeld to pay 20% of the next $50,000 of expenses for this case. After Newfeld's treatment costs on a case reach $70,000, Azalea reimburses the hospital for all subsequent treatment costs.
The maximum amount for which Newfeld is at risk for any one Azalea plan member's treatment costs is
A health plan that capitates a provider group typically provides or offers to provide stop-loss coverage to that provider group.
The Norton Health Plan used blended rating to develop a premium rate for the Roswell Company, a large employer group. Norton assigned Roswell a credibility factor of 0.7 (or 70%). Norton calculated Roswell’s manual rate to be $200 and its experience claims cost as $180. Norton’s retention charge is $3. This information indicates that Roswell’s blended rate is:
For a given healthcare product, the Magnolia Health Plan has a premium of $80 PMPM and a unit variable cost of $30 PMPM. Fixed costs for this product are $30,000 per month. Magnolia can correctly calculate the break-even point for this product to be:
Health plans have access to a variety of funding sources depending on whether they are operated as for-profit or not-for-profit organizations. The Verde Health Plan is a for-profit health plan and the Noir Health Plan is a not-for-profit health plan. From the answer choices below, select the response that correctly identifies whether funds from debt markets and equity markets are available to Verde and Noir:
Companies typically produce three types of budgets: operational budgets, cash budgets, and capital budgets. The following statements are about operational budgets. Select the answer choice containing the correct statement.
The following paragraph contains two pair of terms enclosed in parentheses. Determine which term in each pair correctly completes the statements. Then select the answer choice containing the two terms you have chosen.
In a typical health plan, an (actuary / underwriter) is ultimately responsible for the determination of the appropriate rate to charge for a given level of healthcare benefits and administrative services in a particular market. The (actuary / underwriter) assesses and classifies the degree of risk represented by a proposed group or individual.
The Landau health plan will switch from using top-down budgeting to using bottom-up budgeting. One potential advantage to Landau of making this switch is that, compared to top-down budgeting, bottom-up budgeting is more likely to
The following transactions occurred at the Lane Health Plan:
Transaction 1 — Lane recorded a $25,000 premium prior to receiving the payment
Transaction 2 — Lane purchased $500 in office expenses on account, but did not record the expense until it received the bill a month later
Transaction 3 — Fire destroyed one of Lane’s facilities; Lane waited until the facility was rebuilt before assessing and recording the amount of loss
Transaction 4 — Lane sold an investment on which it realized a $14,000 gain; Lane recorded the gain only after the sale was completed.
Of these transactions, the one that is consistent with the accounting principle of conservatism is:
Analysts will use the capital asset pricing model (CAPM) to determine the cost of equity for the Maxim health plan, a for-profit plan. According to the CAPM, Maxim's cost of equity is equal to
The core of a health plan's strategic financial plan is the development of its pro forma financial statements. The following statements are about these pro forma financial statements. Select the answer choice containing the correct statement.
Residual trend is the difference between total trend and the portion of the total trend caused by changes in provider reimbursement levels.
Consider the following events that could affect an health plan’s provider reimbursement levels:
Event 1 — The disenrollment of a large group with unusually high utilization rates
Event 2 — The introduction of a new treatment for infertility
Event 3 — A serious flu epidemic
Event 4 — A shift in inpatient medical services from obstetrical care to neonatal intensive care
One cause of residual trend is change in intensity, which would be represented by:
The Column health plan is in the process of developing a strategic plan.
The following statements are about this strategic plan. Three of the statements are true, and one statement is false. Select the answer choice containing the FALSE statement.