- Home
- CBIC
- Infection Control
- CIC
- CBIC Certified Infection Control Exam Questions and Answers
CIC CBIC Certified Infection Control Exam Questions and Answers
A patient with a history of Clostridioides difficile is admitted to the hospital. The patient is asymptomatic for diarrheal symptoms; however, the provider prescribes an antibiotic. What type of antimicrobial therapy is applied in this scenario?
Options:
Empiric
Inappropriate
Prophylactic
Targeted
Answer:
CExplanation:
The CBIC Certified Infection Control Exam Study Guide (6th edition) defines prophylactic antimicrobial therapy as the use of antibiotics to prevent infection in the absence of clinical signs or symptoms of active disease. In this scenario, the patient has a history of Clostridioides difficile infection but is currently asymptomatic for diarrhea or other CDI manifestations. The antibiotic is therefore not being used to treat active infection.
Empiric therapy (Option A) is initiated when infection is suspected but the causative organism has not yet been identified—this does not apply here, as the patient has no symptoms suggesting infection. Targeted therapy (Option D) requires laboratory confirmation of a specific pathogen, which is also not present. While prescribing antibiotics in patients with prior CDI may be clinically questionable depending on indication and stewardship principles, the type of therapy being applied is best categorized as prophylactic, not inappropriate, based on standard antimicrobial definitions.
The Study Guide emphasizes that antimicrobial stewardship programs carefully evaluate prophylactic antibiotic use because unnecessary exposure can disrupt normal flora and increase the risk of CDI recurrence. However, from a classification standpoint, antibiotics given without signs of active infection fall under prophylactic use.
For CIC® exam preparation, it is important to correctly identify antimicrobial intent, even when clinical appropriateness may be debatable.
A ventilator-associated pneumonia rate in the ICU has increased from 8.1 infections/1,000 ventilator days to 15.4 infections/1,000 ventilator days over the past two months. To determine the root cause for this increase, the MOST appropriate tool for a performance improvement team is a:
Options:
Fishbone diagram
Pareto chart
Flow diagram
Control chart
Answer:
AExplanation:
The CBIC Certified Infection Control Exam Study Guide (6th edition) identifies the fishbone diagram, also known as a cause-and-effect diagram or Ishikawa diagram, as the most appropriate tool for conducting root cause analysis when investigating an increase in adverse outcomes such as ventilator-associated pneumonia (VAP). This tool is specifically designed to systematically explore multiple contributing factors that may be driving a problem.
A fishbone diagram helps a multidisciplinary performance improvement team organize potential causes into logical categories, commonly including people, processes, equipment, environment, materials, and policies. In the case of rising VAP rates, the team might examine factors such as ventilator care practices, oral hygiene compliance, head-of-bed elevation, sedation practices, staffing levels, equipment maintenance, and adherence to prevention bundles. By visually mapping these contributors, the team can identify underlying system issues rather than focusing on isolated events or individual performance.
The other tools listed are less appropriate for root cause determination. A Pareto chart is useful for prioritizing the most frequent contributors after causes are identified, but it does not identify causes itself. A flow diagram maps process steps but does not analyze why failures occur. A control chart monitors variation over time but does not explain causation.
For CIC® exam preparation, it is essential to recognize that fishbone diagrams are the primary tool for identifying root causes in performance improvement investigations involving increased infection rates.
Healthcare workers are MOST likely to benefit from infection prevention education if the Infection Preventionist (IP)
Options:
brings in speakers who are recognized experts.
plans the educational program well ahead of time.
audits practices and identifies deficiencies.
involves the staff in determining the content.
Answer:
DExplanation:
The correct answer is D, " involves the staff in determining the content, " as this approach is most likely to benefit healthcare workers from infection prevention education. According to the Certification Board of Infection Control and Epidemiology (CBIC) guidelines, effective education programs are tailored to the specific needs and contexts of the learners. Involving staff in determining the content ensures that the educational material addresses their real-world challenges, knowledge gaps, and interests, thereby increasing engagement, relevance, and application of the learned principles (CBIC Practice Analysis, 2022, Domain IV: Education and Research, Competency 4.1 - Develop and implement educational programs). This participatory approach fosters ownership and accountability among healthcare workers, enhancing the likelihood that they will adopt and sustain infection prevention practices.
Option A (brings in speakers who are recognized experts) can enhance credibility and provide high-quality information, but it does not guarantee that the content will meet the specific needs of the staff unless their input is considered. Option B (plans the educational program well ahead of time) is important for logistical success and preparedness, but without staff involvement, the program may lack relevance or fail to address immediate concerns. Option C (audits practices and identifies deficiencies) is a valuable step in identifying areas for improvement, but it is a diagnostic process rather than a direct educational strategy; education based solely on audits might not engage staff effectively if their input is not sought.
The focus on involving staff aligns with CBIC’s emphasis on adult learning principles, which highlight the importance of learner-centered education. By involving staff, the IP adheres to best practices for adult education, ensuring that the program is practical and tailored, ultimately leading to better outcomes in infection prevention (CBIC Practice Analysis, 2022, Domain IV: Education and Research, Competency 4.2 - Evaluate the effectiveness of educational programs). This approach also supports a collaborative culture, which is critical for sustaining infection control efforts in healthcare settings.
During the last week in June, an emergency department log reveals numerous cases of profuse watery diarrhea in individuals 74 years of age and older. During the same time period, four immunocompromised patients were admitted with possible Cryptosporidium. Which of the following actions should the infection preventionist take FIKST?
Options:
Characterize the outbreak by person, place, and time
Increase surveillance facility wide for additional cases
Contact the laboratory to confirm stool identification results
Form a tentative hypothesis about the potential reservoir for this outbreak
Answer:
AExplanation:
When an outbreak of infectious disease is suspected, the first step is to conduct an epidemiologic investigation. This begins with characterizing the outbreak by person, place, and time to establish patterns and trends. This approach, known as descriptive epidemiology, provides critical insights into potential sources and transmission patterns.
Step-by-Step Justification:
Identify Cases and Patterns:
The infection preventionist should analyze patient demographics (person), locations of cases (place), and onset of symptoms (time). This helps in defining the outbreak scope and potential exposure sources.
Create an Epidemic Curve:
An epidemic curve helps determine whether the outbreak is a point-source or propagated event. This can indicate whether the infection is spreading person-to-person or originating from a common source.
Compare with Baseline Data:
Reviewing historical data ensures that the observed cases exceed the expected norm, confirming an outbreak.
Guide Further Investigation:
Establishing basic epidemiologic patterns guides subsequent actions, such as laboratory testing, environmental sampling, and surveillance.
Why Other Options Are Incorrect:
B. Increase surveillance facility-wide for additional cases:
While enhanced surveillance is important, it should follow the initial characterization of the outbreak. Surveillance without a defined case profile may lead to misclassification and misinterpretation.
C. Contact the laboratory to confirm stool identification results:
Confirming lab results is essential but comes after defining the outbreak ' s characteristics. Without an epidemiologic link, testing may yield results that are difficult to interpret.
D. Form a tentative hypothesis about the potential reservoir for this outbreak:
Hypothesis generation occurs after sufficient epidemiologic data have been collected. Jumping to conclusions without characterization may result in incorrect assumptions and ineffective control measures.
CBIC Infection Control References:
APIC Text, " Outbreak Investigations, " Epidemiology, Surveillance, Performance, and Patient Safety Measures.
APIC/JCR Infection Prevention and Control Workbook, Chapter 4, Surveillance Program.
APIC Text, " Investigating Infectious Disease Outbreaks, " Guidelines for Epidemic Curve Analysis.
A hospital is experiencing an increase in vancomycin-resistant Enterococcus (VRE) infections in the hematology-oncology unit. Which of the following interventions is MOST effective in halting the spread of VRE in this high-risk setting?
Options:
Screening all patients on admission and placing positive patients in isolation.
Restricting the use of vancomycin for all patients in the hospital.
Implementing a hand hygiene compliance audit and feedback system.
Conducting environmental sampling for VRE contamination weekly.
Answer:
CExplanation:
Comprehensive and Detailed In-Depth Explanation:
Hand hygiene remains the single most effective intervention to prevent the spread of vancomycin-resistant Enterococcus (VRE) in healthcare settings. Implementing an audit and feedback system significantly improves compliance and reduces VRE transmission.
Step-by-Step Justification:
Hand Hygiene Compliance Audit and Feedback (Best Strategy)
Studies show that poor hand hygiene is the primary mode of VRE transmission in hospitals.
Implementing real-time auditing with feedback ensures sustained compliance and helps identify weak areas.
Why Other Options Are Incorrect:
A. Screening all patients and isolating VRE-positive patients:
While screening helps identify carriers, contact precautions alone are not sufficient without strong hand hygiene enforcement.
B. Restricting vancomycin use:
While antimicrobial stewardship is crucial, vancomycin use alone does not drive VRE outbreaks—poor infection control practices do.
D. Conducting environmental sampling weekly:
Routine sampling is not necessary; immediate terminal disinfection and improved hand hygiene are more effective.
CBIC Infection Control References:
APIC Text, " VRE Prevention and Hand Hygiene, " Chapter 11.
APIC-JCR Workbook, " Antimicrobial Resistance and Infection Control Measures, " Chapter 7.
Which of the following strategies is MOST effective in reducing surgical site infections (SSI) in orthopedic procedures?
Options:
Perioperative normothermia maintenance.
Routine intraoperative wound irrigation with povidone-iodine.
Administration of prophylactic antibiotics postoperatively for 48 hours.
Use of sterile adhesive wound dressings for 10 days postoperatively.
Answer:
AExplanation:
Perioperative normothermia maintenance reduces SSI rates by improving immune function and tissue perfusion.
Routine wound irrigation (B) has no strong evidence supporting SSI prevention.
Prolonged antibiotic use (C) increases antibiotic resistance without added benefit.
Extended use of wound dressings (D) does not reduce SSI rates.
CBIC Infection Control References:
APIC Text, " SSI Prevention in Surgery, " Chapter 12.
The infection preventionist (IP) is assisting pharmacists in investigating medication contamination at the hospital’s compounding pharmacy. As part of the medication recall process, the IP should:
Options:
Have laboratory culture all medication.
Inspect for safe injection practices.
Identify the potential source of contamination.
Inform all discharged patients of potential medication contamination.
Answer:
CExplanation:
The scenario involves an infection preventionist (IP) assisting pharmacists in addressing medication contamination at the hospital’s compounding pharmacy, with a focus on the medication recall process. The IP’s role is to apply infection control expertise to mitigate risks, guided by the Certification Board of Infection Control and Epidemiology (CBIC) principles and best practices. The recall process requires a systematic approach to identify, contain, and resolve the issue, and the “first” or most critical step must be determined. Let’s evaluate each option:
A. Have laboratory culture all medication: Culturing all medication to confirm contamination is a valuable step to identify affected batches and guide the recall. However, this is a resource-intensive process that depends on first understanding the scope and source of the problem. Without identifying the potential source of contamination, culturing all medication could be inefficient and delay the recall. This step is important but secondary to initial investigation.
B. Inspect for safe injection practices: Inspecting for safe injection practices (e.g., single-use vials, proper hand hygiene, sterile technique) is a critical infection control measure, especially in compounding pharmacies where contamination often arises from procedural errors (e.g., reuse of syringes, improper cleaning). While this is a proactive step to prevent future contamination, it addresses ongoing practices rather than the immediate recall process for the current contamination event. It is a complementary action but not the first priority.
C. Identify the potential source of contamination: Identifying the potential source of contamination is the foundational step in the recall process. This involves investigating the compounding environment (e.g., water quality, equipment, personnel practices), raw materials, and production processes to pinpoint where the contamination occurred (e.g., bacterial ingress, cross-contamination). The CBIC emphasizes root cause analysis as a key infection prevention strategy, enabling targeted recalls, corrective actions, and prevention of recurrence. This step is essential before culturing, inspecting, or notifying patients, making it the IP’s primary responsibility in this context.
D. Inform all discharged patients of potential medication contamination: Notifying patients is a critical step to ensure public safety and allow for medical follow-up if they received contaminated medication. However, this action requires prior identification of the contaminated batches and their distribution, which depends on determining the source and confirming the extent of the issue. Premature notification without evidence could cause unnecessary alarm and is not the first step in the recall process.
The best answer is C, as identifying the potential source of contamination is the initial and most critical step in the medication recall process. This allows the IP to collaborate with pharmacists to trace the contamination, define the affected products, and guide subsequent actions (e.g., culturing, inspections, notifications). This aligns with CBIC’s focus on systematic investigation and risk mitigation in healthcare-associated infection events.
CBIC Infection Prevention and Control (IPC) Core Competency Model (updated 2023), Domain III: Prevention and Control of Infectious Diseases, which includes identifying sources of contamination in healthcare settings.
CBIC Examination Content Outline, Domain V: Management and Communication, which emphasizes root cause analysis during outbreak investigations.
CDC Guidelines for Safe Medication Compounding (2022), which recommend identifying contamination sources as the first step in a recall process.
Which of the following products or methods is effective for sterilization of heat-sensitive critical items?
Options:
Phenolics
Chlorine-based
Quaternary ammonium
Hydrogen peroxide gas plasma
Answer:
DExplanation:
The CBIC Certified Infection Control Exam Study Guide (6th edition) explains that critical items—those that enter sterile tissue or the vascular system—must be sterile at the time of use. When these items are heat-sensitive and cannot tolerate steam sterilization, low-temperature sterilization technologies are required. Among the options listed, hydrogen peroxide gas plasma is an FDA-cleared, low-temperature sterilization method specifically designed for heat- and moisture-sensitive medical devices.
Hydrogen peroxide gas plasma sterilization achieves sterilization by generating reactive free radicals that destroy microorganisms, including bacteria, viruses, fungi, and spores. The study guide emphasizes that this method provides true sterilization rather than disinfection and is widely used for delicate instruments such as certain endoscopes, optical devices, and electronic equipment. It also offers advantages such as short cycle times and minimal toxic residues.
The other options are incorrect because they do not achieve sterilization. Phenolics, chlorine-based products, and quaternary ammonium compounds are disinfectants, not sterilants, and are inappropriate for critical items. Even at high concentrations, these agents cannot reliably destroy bacterial spores and therefore do not meet the definition of sterilization.
This question highlights a key CIC exam concept: critical items require sterilization, and when heat cannot be used, approved low-temperature sterilization technologies such as hydrogen peroxide gas plasma are required to ensure patient safety.
Each item or package that is prepared for sterilization should be labeled with the
Options:
storage location.
type of sterilization process.
sterilizer identification number or code.
cleaning method (e.g., mechanical or manual).
Answer:
CExplanation:
The correct answer is C, " sterilizer identification number or code, " as this is the essential information that each item or package prepared for sterilization should be labeled with. According to the Certification Board of Infection Control and Epidemiology (CBIC) guidelines, proper labeling of sterilized items is a critical component of infection prevention and control to ensure traceability and verify the sterilization process. The sterilizer identification number or code links the item to a specific sterilization cycle, allowing the infection preventionist (IP) and sterile processing staff to track the equipment used, confirm compliance with standards (e.g., AAMI ST79), and facilitate recall or investigation if issues arise (CBIC Practice Analysis, 2022, Domain III: Infection Prevention and Control, Competency 3.3 - Ensure safe reprocessing of medical equipment). This labeling ensures that the sterility of the item can be assured and documented, protecting patient safety by preventing the use of inadequately processed items.
Option A (storage location) is important for inventory management but is not directly related to the sterilization process itself and does not provide evidence of the sterilization event. Option B (type of sterilization process) indicates the method (e.g., steam, ethylene oxide), which is useful but less critical than the sterilizer identification, as the process type alone does not confirm the specific cycle or equipment used. Option D (cleaning method, e.g., mechanical or manual) is a preliminary step in reprocessing, but it is not required on the sterilization label, as the focus shifts to sterilization verification once the item is prepared.
The requirement for a sterilizer identification number or code aligns with CBIC’s emphasis on maintaining rigorous tracking and quality assurance in the reprocessing of medical devices, ensuring accountability and adherence to best practices (CBIC Practice Analysis, 2022, Domain III: Infection Prevention and Control, Competency 3.5 - Evaluate the environment for infection risks). This practice is mandated by standards such as AAMI ST79 to support effective infection control in healthcare settings.
Which of the following processes is MOST important for the infection preventionist (IP) to review when evaluating a third-party reprocessor for single-use devices?
Options:
Observe all steps for reprocessing.
Review the facility ' s blueprints and policies.
Ensure air and water cultures are performed regularly.
Obtain feedback from other IPs who use the reprocessor.
Answer:
AExplanation:
The correct answer is A, " Observe all steps for reprocessing, " as this is the most important process for the infection preventionist (IP) to review when evaluating a third-party reprocessor for single-use devices. According to the Certification Board of Infection Control and Epidemiology (CBIC) guidelines, the reprocessing of single-use devices (SUDs) by third-party entities must adhere to stringent infection control standards to ensure they are safe for reuse and do not contribute to healthcare-associated infections (HAIs). Observing all steps—such as cleaning, disinfection, sterilization, packaging, and quality control—allows the IP to directly assess compliance with manufacturer instructions, regulatory requirements (e.g., FDA guidelines), and best practices (e.g., AAMI ST91) (CBIC Practice Analysis, 2022, Domain III: Infection Prevention and Control, Competency 3.3 - Ensure safe reprocessing of medical equipment). This hands-on evaluation is critical because any deviation in the reprocessing chain can compromise device sterility and patient safety.
Option B (review the facility ' s blueprints and policies) provides context about the physical layout and procedural framework, but it is a preliminary step that does not directly verify the reprocessing process’s effectiveness. Option C (ensure air and water cultures are performed regularly) is important for monitoring environmental contamination risks, particularly in sterile processing areas, but it is a supportive measure rather than the primary focus of evaluating the reprocessor’s core activities. Option D (obtain feedback from other IPs who use the reprocessor) offers valuable peer insights, but it is subjective and secondary to direct observation, which provides firsthand evidence of compliance and performance.
The priority on observing reprocessing steps aligns with CBIC’s emphasis on ensuring the safety and efficacy of reprocessed medical devices, a key responsibility for IPs when outsourcing to third-party reprocessors (CBIC Practice Analysis, 2022, Domain III: Infection Prevention and Control, Competency 3.5 - Evaluate the environment for infection risks). This process enables the IP to identify specific weaknesses, validate adherence to standards, and make informed decisions about the reprocessor’s suitability.
The MOST common route of infection for healthcare-associated (HA) pneumonia is:
Options:
Aspiration of bacteria from the oropharynx
Person-to-person spread from healthcare personnel’s (HCP) hands
Contamination from small-volume nebulizers
Droplet inhalation from large-volume humidifiers
Answer:
AExplanation:
The CBIC Certified Infection Control Exam Study Guide (6th edition) identifies aspiration of bacteria from the oropharynx as the most common route of infection for healthcare-associated pneumonia, including hospital-acquired pneumonia (HAP) and ventilator-associated pneumonia (VAP). In hospitalized patients—especially those who are critically ill, sedated, intubated, or have impaired consciousness—the normal defense mechanisms that prevent aspiration are compromised.
Colonization of the oropharynx with pathogenic organisms occurs rapidly in hospitalized patients due to factors such as antibiotic exposure, underlying illness, poor oral hygiene, and use of invasive devices. Microaspiration of contaminated oral and gastric secretions into the lower respiratory tract is a frequent event and represents the primary mechanism by which pathogens reach the lungs. This risk is significantly increased in patients receiving mechanical ventilation or those positioned supine.
The other options represent less common routes. Transmission from healthcare personnel hands (Option B) contributes indirectly by facilitating colonization but is not the primary route of pneumonia development. Contaminated nebulizers (Option C) and humidifiers (Option D) have been associated with outbreaks but are now uncommon causes due to improved equipment design and maintenance practices.
For CIC® exam preparation, it is essential to recognize that preventive strategies for HA pneumonia focus heavily on reducing aspiration risk, including head-of-bed elevation, oral care protocols, and minimizing sedation—directly addressing the most common route of infection.
A director of the Infection Prevention and Control Department has received permission to hire more staff to a total of 3.8 full-time equivalents (FTEs), based on 40 hours/week. The director works 40 hours/week, one infection preventionist (IP) works 32 hours/week, another works 16 hours/week, and secretarial support works 40 hours/week. How many additional FTEs may the director hire?
Options:
0.4
0.6
0.8
1.0
Answer:
BExplanation:
The Certification Study Guide (6th edition) stresses that infection prevention leaders must understand basic workforce and FTE calculations to ensure appropriate staffing and compliance with approved resource allocations. An FTE is defined as 40 hours worked per week, and part-time hours must be converted proportionally.
First, calculate the FTEs already in use:
Director: 40 hours/week ÷ 40 = 1.0 FTE
Infection preventionist: 32 hours/week ÷ 40 = 0.8 FTE
Infection preventionist: 16 hours/week ÷ 40 = 0.4 FTE
Secretarial support: 40 hours/week ÷ 40 = 1.0 FTE
Total current FTEs:
1.0 + 0.8 + 0.4 + 1.0 = 3.2 FTEs
The approved staffing total is 3.8 FTEs. To determine how many additional FTEs may be hired, subtract current FTE usage from the approved total:
3.8 − 3.2 = 0.6 FTE
Therefore, the director may hire 0.6 additional FTE, which could be fulfilled by a part-time infection preventionist or split among staff roles, depending on organizational needs.
CIC exam questions frequently test practical management skills, including staffing calculations, budgeting awareness, and resource allocation. Accurate FTE calculations ensure compliance with administrative approvals and support safe, effective infection prevention program operations.
Which of the following blood-drawing methods is considered to be a needle-safe practice?
Options:
Use a syringe with a needle attached.
Shielded needles for vacuum-tube phlebotomy sets.
Remove contaminated needles from blood collection sets.
Inject blood into vacuum tubes using conventional syringes.
Answer:
BExplanation:
The CBIC Certified Infection Control Exam Study Guide (6th edition) identifies engineered sharps injury prevention devices (ESIPDs) as the cornerstone of needle-safe practices during blood collection. Shielded needles used with vacuum-tube phlebotomy systems are specifically designed to reduce the risk of needlestick injuries by incorporating a built-in safety mechanism that covers or retracts the needle immediately after use.
Vacuum-tube systems with shielded needles allow blood to flow directly into collection tubes without the need for needle removal or blood transfer, thereby minimizing handling of sharps. Once blood collection is complete, the safety feature is activated—often automatically or with a single-handed technique—significantly reducing exposure risk to healthcare personnel. The Study Guide emphasizes that these devices meet regulatory expectations under the Needlestick Safety and Prevention Act and should be used whenever feasible.
The other options are unsafe practices. Using syringes with attached needles (Option A) increases risk during transfer and disposal. Removing contaminated needles from collection sets (Option C) is explicitly prohibited due to high injury risk. Injecting blood into vacuum tubes using conventional syringes (Option D) requires manipulating exposed needles and increases the likelihood of splashes and sharps injuries.
For CIC® exam preparation, it is essential to recognize that needle-safe blood collection relies on safety-engineered devices, with shielded vacuum-tube phlebotomy needles representing best practice for preventing occupational exposures.
Which of the following represents a class II surgical wound?
Options:
Incisions in which acute, nonpurulent inflammation are seen.
Incisional wounds following nonpenetrating (blunt) trauma.
Incisions involving the biliary tract, appendix, vagina, and oropharynx.
Old traumatic wounds with retained devitalized tissue.
Answer:
AExplanation:
Surgical wounds are classified by the Centers for Disease Control and Prevention (CDC) into four classes based on the degree of contamination and the likelihood of postoperative infection. This classification system, detailed in the CDC’s Guidelines for Prevention of Surgical Site Infections (1999), is a cornerstone of infection prevention and control, aligning with the Certification Board of Infection Control and Epidemiology (CBIC) standards in the " Prevention and Control of Infectious Diseases " domain. The classes are as follows:
Class I (Clean): Uninfected operative wounds with no inflammation, typically closed primarily, and not involving the respiratory, alimentary, genital, or urinary tracts.
Class II (Clean-Contaminated): Operative wounds with controlled entry into a sterile or minimally contaminated tract (e.g., biliary or gastrointestinal), with no significant spillage or infection present.
Class III (Contaminated): Open, fresh wounds with significant spillage (e.g., from a perforated viscus) or major breaks in sterile technique.
Class IV (Dirty-Infected): Old traumatic wounds with retained devitalized tissue or existing clinical infection.
Option A, " Incisions in which acute, nonpurulent inflammation are seen, " aligns with a Class II surgical wound. The presence of acute, nonpurulent inflammation suggests a controlled inflammatory response without overt infection, which can occur in clean-contaminated cases where a sterile tract (e.g., during elective gastrointestinal surgery) is entered under controlled conditions. The CDC defines Class II wounds as those involving minor contamination without significant spillage or infection, and nonpurulent inflammation fits this category, often seen in early postoperative monitoring.
Option B, " Incisional wounds following nonpenetrating (blunt) trauma, " does not fit the Class II definition. These wounds are typically classified based on the trauma context and are more likely to be considered contaminated (Class III) or dirty (Class IV) if there is tissue damage or delayed treatment, rather than clean-contaminated. Option C, " Incisions involving the biliary tract, appendix, vagina, and oropharynx, " describes anatomical sites that, when surgically accessed, often fall into Class II if the procedure is elective and controlled (e.g., cholecystectomy), but the phrasing suggests a general category rather than a specific wound state with inflammation, making it less precise for Class II. Option D, " Old traumatic wounds with retained devitalized tissue, " clearly corresponds to Class IV (dirty-infected) due to the presence of necrotic tissue and potential existing infection, which is inconsistent with Class II.
The CBIC Practice Analysis (2022) emphasizes the importance of accurate wound classification for implementing appropriate infection prevention measures, such as antibiotic prophylaxis or sterile technique adjustments. The CDC guidelines further specify that Class II wounds may require tailored interventions based on the observed inflammatory response, supporting Option A as the correct answer. Note that the phrasing in Option A contains a minor grammatical error ( " inflammation are seen " should be " inflammation is seen " ), but this does not alter the clinical intent or classification.
Which of the following organisms is associated with a waterborne disease?
Options:
Bacillus anthracis
Cytomegalovirus
Nontuberculous mycobacteria
Stachybotrys
Answer:
CExplanation:
The CBIC Certified Infection Control Exam Study Guide (6th edition) identifies nontuberculous mycobacteria (NTM) as organisms commonly associated with waterborne exposure. NTM are environmental mycobacteria widely found in natural and treated water sources, including potable water systems, ice machines, showerheads, faucets, and medical equipment rinsed with tap water. Because these organisms are resistant to standard water disinfection methods and can form biofilms, they are particularly well adapted to survive in plumbing systems.
NTM have been implicated in healthcare-associated infections, especially among immunocompromised patients, and may cause pulmonary disease, skin and soft tissue infections, and invasive disease following exposure to contaminated water or medical devices. The Study Guide emphasizes the importance of water management programs and routine surveillance to prevent waterborne transmission of opportunistic pathogens such as NTM and Legionella.
The other answer options are incorrect. Bacillus anthracis is primarily associated with zoonotic and bioterrorism-related exposure, not waterborne transmission. Cytomegalovirus is transmitted through direct contact with bodily fluids rather than water. Stachybotrys is a mold associated with damp indoor environments but is not considered a waterborne pathogen in the context of infection transmission.
Understanding organisms linked to water systems is critical for infection preventionists, as waterborne pathogens present ongoing risks in healthcare facilities and are a key topic on the CIC® exam.
==========
What rate is expressed by the number of patients who acquire infections over a specified time period divided by the population at risk of acquiring an infection during that time period?
Options:
Incidence rate
Disease specific
Point prevalence
Period prevalence
Answer:
AExplanation:
The incidence rate measures new cases of infection in a population over a defined time period using the formula:
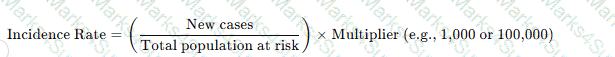
Why the Other Options Are Incorrect?
B. Disease specific – Refers to infections caused by a particular pathogen, not the general rate of new infections.
C. Point prevalence – Measures existing cases at a specific point in time, not new cases.
D. Period prevalence – Includes both old and new cases over a set period, unlike incidence, which only considers new cases.
CBIC Infection Control Reference
APIC defines incidence rate as the number of new infections in a population over a given period.
Given the formula for calculating incidence rates, the Y represents which of the following?

Options:
Population served
Number of infected patients
Population at risk
Number of events
Answer:
CExplanation:
Incidence rate is a fundamental epidemiological measure used to quantify the frequency of new cases of a disease within a specified population over a defined time period. The Certification Board of Infection Control and Epidemiology (CBIC) supports the use of such metrics in the " Surveillance and Epidemiologic Investigation " domain, aligning with the Centers for Disease Control and Prevention (CDC) " Principles of Epidemiology in Public Health Practice " (3rd Edition, 2012). The formula provided, XY×K=Rate\frac{X}{Y} \times K = RateYX×K=Rate, represents the standard incidence rate calculation, where KKK is a constant (e.g., 1,000 or 100,000) to express the rate per unit population, and the question asks what YYY represents among the given options.
In the incidence rate formula, XXX typically represents the number of new cases (or events) of the disease occurring during a specific period, and YYY represents the population at risk during that same period. The ratio XY\frac{X}{Y}YX yields the rate per unit of population, which is then multiplied by KKK to standardize the rate (e.g., cases per 1,000 persons). The CDC defines the denominator (YYY) as the population at risk, which includes individuals susceptible to the disease over the observation period. Option B ( " Number of infected patients " ) might suggest XXX if it specified new cases, but as the denominator YYY, it is incorrect because incidence focuses on new cases relative to the at-risk population, not the total number of infected individuals (which could include prevalent cases). Option C ( " Population at risk " ) correctly aligns with YYY, representing the base population over which the rate is calculated.
Option A, " Population served, " is a broader term that might include the total population under care (e.g., in a healthcare facility), but it is not specific to those at risk for new infections, making it less precise. Option D, " Number of events, " could align with XXX (new cases or events), but as the denominator YYY, it does not fit the formula’s structure. The CBIC Practice Analysis (2022) and CDC guidelines reinforce that the denominator in incidence rates is the population at risk, ensuring accurate measurement of new disease occurrence.
An infection preventionist is reviewing practices in a facility ' s food preparation department. Which of the following practices should be revised?
Options:
Thawing meat at room temperature
Using a cutting board to cut vegetables
Maintaining hot food at 145° F (62.7° C) during serving
Discarding most perishable food within 72 hours
Answer:
AExplanation:
Thawing raw meat at room temperature is a major food safety violation because it allows bacteria to multiply rapidly within the temperature danger zone (40–140°F or 4.4–60°C). Meat should always be thawed in the refrigerator, under cold running water, or in a microwave if cooked immediately.
Why the Other Options Are Incorrect?
B. Using a cutting board to cut vegetables – This is safe as long as proper cleaning and sanitation procedures are followed.
C. Maintaining hot food at 145°F (62.7°C) during serving – 145°F is an acceptable minimum temperature for certain meats like beef, fish, and pork.
D. Discarding most perishable food within 72 hours – Many perishable foods, especially leftovers, should be discarded within 3 days, making this an appropriate practice.
CBIC Infection Control Reference
The APIC guidelines emphasize that raw meat should never be thawed at room temperature due to the risk of bacterial growth and foodborne illness.
A nutrition support team wants to determine whether patients who receive total parenteral nutrition (TPN) at home are at increased risk of central line–associated bloodstream infection (CLABSI) compared with patients who receive TPN in the hospital. The BEST way to compare these two groups is to calculate the:
Options:
Percentage of patients in each group who became infected.
Infections per 1,000 central line days in each group.
Number of infections in each group this year compared to last year.
Ratio of infected to noninfected central lines in each group.
Answer:
BExplanation:
The CBIC Certified Infection Control Exam Study Guide (6th edition) emphasizes that accurate comparison of healthcare-associated infection risk between groups requires use of standardized, exposure-based rates. For central line–associated bloodstream infections (CLABSIs), the recommended metric is infections per 1,000 central line days, which accounts for the amount of time patients are actually exposed to the risk factor—in this case, the presence of a central venous catheter.
Patients receiving TPN at home and those receiving TPN in the hospital may differ substantially in duration of catheter use, care practices, and patient acuity. Simply comparing percentages or raw numbers of infections fails to adjust for differences in central line utilization and can result in misleading conclusions. By using central line days as the denominator, infection rates are normalized and allow for valid comparisons between populations and settings.
Option A does not account for differences in exposure time. Option C compares different time periods rather than comparing risk between groups. Option D provides a ratio but lacks standardization and is not consistent with accepted surveillance methodology.
The Study Guide reinforces that device-associated infection surveillance—such as CLABSI monitoring—must use device days to assess true risk and guide prevention strategies. Understanding and applying correct epidemiologic measures is a core competency for infection preventionists and a frequently tested concept on the CIC® exam.
==========
What data should be collected and analyzed as part of a syndromic surveillance program?
Options:
Number of blood and urine cultures
Number of visits to physical therapy
Number of surgical procedures performed
Number of over-the-counter sales of flu remedies
Answer:
DExplanation:
The Certification Study Guide (6th edition) describes syndromic surveillance as a public health surveillance approach that focuses on the early detection of disease outbreaks by monitoring nonspecific indicators that precede formal diagnosis or laboratory confirmation. Rather than relying on confirmed cases, syndromic surveillance tracks patterns of symptoms, behaviors, or indirect data sources that may signal emerging health threats.
One key example emphasized in the study guide is the monitoring of over-the-counter (OTC) medication sales, such as flu and cold remedies. Increases in OTC sales can indicate a rise in respiratory illness within the community before patients seek medical care or receive laboratory testing. This early signal allows infection preventionists and public health officials to initiate investigations, preparedness measures, and targeted messaging sooner than traditional surveillance methods would allow.
The other options reflect data used in traditional or outcome-based surveillance, not syndromic surveillance. Blood and urine cultures require laboratory confirmation and occur later in the disease process. Physical therapy visits and surgical procedure counts are unrelated to early symptom detection and do not provide timely indicators of infectious disease trends.
CIC exam questions frequently test the distinction between traditional surveillance and syndromic surveillance. Recognizing that syndromic surveillance relies on early, indirect indicators of illness, such as OTC medication sales, is essential for accurate exam performance and effective outbreak preparedness.
What antimicrobial is associated with increased Clostridioides difficile infection?
Options:
Amoxicillin
Aztreonam
Clindamycin
Tobramycin
Answer:
CExplanation:
The CBIC Certified Infection Control Exam Study Guide (6th edition) identifies clindamycin as one of the antimicrobials most strongly associated with an increased risk of Clostridioides difficile infection (CDI). Clindamycin has a profound impact on the normal intestinal microbiota, significantly disrupting protective gut flora that ordinarily suppress C. difficile overgrowth. This disruption creates an environment conducive to colonization and toxin production by C. difficile, leading to clinical infection.
Historically, clindamycin was one of the first antibiotics clearly linked to large outbreaks of CDI, and it remains a high-risk agent today. The Study Guide notes that antibiotics with broad anaerobic coverage—including clindamycin, fluoroquinolones, third-generation cephalosporins, and carbapenems—are particularly associated with CDI because they extensively alter gastrointestinal microbial balance.
The other options listed carry comparatively lower risk. Amoxicillin has a modest association but is not among the highest-risk agents. Aztreonam has limited anaerobic activity and is less disruptive to gut flora. Tobramycin, an aminoglycoside, has minimal impact on intestinal microbiota when administered parenterally and is not commonly associated with CDI.
Recognizing high-risk antimicrobials is essential for antimicrobial stewardship, CDI prevention strategies, and CIC® exam success. Clindamycin is classically tested and should be readily identified as a major CDI risk factor.
A nurse exposed to pertussis develops a mild cough 14 days later. What is the recommended action?
Options:
Continue working with a surgical mask.
Exclude from patient care until five days after starting antibiotics.
Initiate post-exposure prophylaxis only if symptoms worsen.
Conduct serologic testing before deciding on work restrictions.
Answer:
BExplanation:
The CDC recommends exclusion of healthcare workers with pertussis until completing at least five days of antibiotic therapy.
CBIC Infection Control References:
APIC-JCR Workbook, " Occupational Health Considerations, " Chapter 10
When describing the differences between colonization and infection, the infection preventionist should define colonization as
Options:
Tissue invasion by organisms without tissue damage.
Tissue injury by normal flora associated with local reaction.
The presence and growth of organisms without tissue invasion.
The presence and growth of opportunistic organisms with cellular change.
Answer:
CExplanation:
The CBIC Certified Infection Control Exam Study Guide (6th edition) clearly distinguishes colonization from infection, a foundational concept in infection prevention and healthcare epidemiology. Colonization is defined as the presence and multiplication of microorganisms on or within a host without tissue invasion, damage, or clinical signs of disease. Individuals who are colonized do not exhibit symptoms and typically do not mount an inflammatory response.
Option C accurately reflects this definition and is the correct answer. Colonized organisms may be part of normal flora or may be potentially pathogenic organisms such as Staphylococcus aureus or multidrug-resistant organisms. Although colonization does not cause illness, colonized individuals can serve as reservoirs for transmission and may later develop infection if host defenses are compromised.
Option A is incorrect because tissue invasion, even without visible damage, represents infection rather than colonization. Option B describes infection caused by normal flora with an inflammatory response. Option D includes cellular change, which indicates tissue response and therefore infection.
For the CIC® exam, it is essential to understand that colonization involves microbial presence without host response, while infection requires tissue invasion and a corresponding inflammatory or immune reaction. This distinction is critical for surveillance definitions, isolation decisions, antimicrobial stewardship, and patient education.
A suspected measles case has been identified in an outpatient clinic without an airborne infection isolation room (AIIR). Which of the following is the BEST course of action?
Options:
Patient should be sent home
Staff should don a respirator, gown, and face shield.
Patient should be offered the Measles. Mumps, Rubella (MMR) vaccine
Patient should be masked and placed in a private room with door closed.
Answer:
DExplanation:
Measles is a highly contagious airborne disease, and the best immediate action in an outpatient clinic without an Airborne Infection Isolation Room (AIIR) is to mask the patient and isolate them in a private room with the door closed.
Why the Other Options Are Incorrect?
A. Patient should be sent home – While home isolation may be necessary, sending the patient home without proper precautions increases exposure risk.
B. Staff should don a respirator, gown, and face shield – While N95 respirators are necessary for staff, this does not address patient containment.
C. Patient should be offered the MMR vaccine – The vaccine does not treat active measles infection and should be given only as post-exposure prophylaxis to susceptible contacts.
CBIC Infection Control Reference
Measles cases in outpatient settings require immediate airborne precautions to prevent transmission.
An infection preventionist (IP) is tasked with developing an infection prevention training program for family members. What step should the IP take FIRST?
Options:
Assess the needs of the family members at the facility.
Create clearly defined goals and objectives for the training.
Ensure that all content in the training is relevant and practical.
Develop a plan to create an appropriate training environment.
Answer:
AExplanation:
The correct answer is A, " Assess the needs of the family members at the facility, " as this is the first step the infection preventionist (IP) should take when developing an infection prevention training program for family members. According to the Certification Board of Infection Control and Epidemiology (CBIC) guidelines, effective education programs begin with a needs assessment to identify the specific knowledge gaps, cultural factors, and practical challenges of the target audience—in this case, family members. This initial step ensures that the training is tailored to their level of understanding, language preferences, and the infection risks they may encounter (e.g., hand hygiene, isolation protocols), aligning with adult learning principles (CBIC Practice Analysis, 2022, Domain IV: Education and Research, Competency 4.1 - Develop and implement educational programs). Without this assessment, subsequent steps risk being misaligned with the audience’s needs, reducing the program’s effectiveness.
Option B (create clearly defined goals and objectives for the training) is a critical step but follows the needs assessment, as goals should be based on identified needs to ensure relevance. Option C (ensure that all content in the training is relevant and practical) depends on understanding the audience’s needs first, making it a later step in the development process. Option D (develop a plan to create an appropriate training environment) is important for implementation but requires prior knowledge of the audience and content to design effectively.
The focus on assessing needs aligns with CBIC’s emphasis on evidence-based education design, enabling the IP to address specific infection prevention priorities for family members and improve outcomes in the facility (CBIC Practice Analysis, 2022, Domain IV: Education and Research, Competency 4.2 - Evaluate the effectiveness of educational programs). This approach is supported by CDC guidelines, which recommend audience assessment as a foundational step in health education programs.
Which event increases a susceptible person’s probability of an infection after an exposure?
Options:
Prior immunization for Hepatitis B virus
An unknown concentration of infectious virions from a needlestick
Healthcare personnel’s (HCP) clothing exposed to the patient’s bodily fluids
A splash of the patient’s blood landing on intact skin on a healthcare personnel’s (HCP) arm
Answer:
BExplanation:
The Certification Study Guide (6th edition) explains that the probability of infection after an exposure is influenced by several factors, including the dose of the infectious agent, the route of exposure, and host susceptibility. Among the options provided, an unknown concentration of infectious virions introduced via a needlestick injury represents the greatest increase in infection risk.
Percutaneous injuries, such as needlesticks, provide direct access to the bloodstream, bypassing natural protective barriers like intact skin. The study guide emphasizes that when the inoculum (number of organisms) is unknown, particularly in bloodborne exposures, the risk of transmission for pathogens such as hepatitis B virus, hepatitis C virus, and human immunodeficiency virus is significantly higher. This uncertainty necessitates immediate evaluation and consideration of post-exposure prophylaxis.
The other options describe situations with lower or reduced risk. Prior immunization for hepatitis B is protective and therefore decreases susceptibility. Exposure of clothing alone does not constitute a significant transmission route unless there is penetration to skin or mucous membranes. Blood splashes onto intact skin are considered low-risk because intact skin acts as an effective barrier against infection.
CIC exam questions frequently test understanding of exposure routes and inoculum size. Recognizing that percutaneous exposure with an unknown infectious dose poses the highest risk is essential for accurate risk assessment and appropriate occupational health response.
A patient with pertussis can be removed from Droplet Precautions after
Options:
direct fluorescent antibody and/or culture are negative.
five days of appropriate antibiotic therapy.
the patient has been given pertussis vaccine.
the paroxysmal stage has ended.
Answer:
BExplanation:
A patient with pertussis (whooping cough) should remain on Droplet Precautions to prevent transmission. According to APIC guidelines, patients with pertussis can be removed from Droplet Precautions after completing at least five days of appropriate antimicrobial therapy and showing clinical improvement.
Why the Other Options Are Incorrect?
A. Direct fluorescent antibody and/or culture are negative – Laboratory results may not always detect pertussis early, and false negatives can occur.
C. The patient has been given pertussis vaccine – The vaccine prevents but does not treat pertussis, and it does not shorten the period of contagiousness.
D. The paroxysmal stage has ended – The paroxysmal stage (severe coughing fits) can last weeks, but infectiousness decreases with antibiotics.
CBIC Infection Control Reference
According to APIC guidelines, Droplet Precautions should continue until the patient has received at least five days of antimicrobial therapy.
An infection preventionist has been informed that a patient admitted 2 days ago has been diagnosed with chickenpox. Ten employees have had contact with this patient. Those employees with significant exposure may be furloughed after exposure. " Significant exposure " is considered
Options:
greater than one hour of direct patient contact occurring within 24 hours prior to the appearance of lesions.
sharing the same air space for any duration of time after the patient has developed skin lesions.
unprotected contact with respiratory secretions or skin lesions occurring after 12 hours of the appearance of lesions.
irrelevant unless the employee has a negative varicella antibody titer.
Answer:
BExplanation:
Chickenpox (varicella) is primarily spread through airborne transmission, and exposure is defined by being in the same airspace with a contagious person (from 1-2 days before rash onset until lesions are crusted), even if briefly.
The APIC Text states:
“Significant exposure is defined as being in the same room or airspace during the period of infectivity, regardless of duration”.
This reflects airborne precaution definitions and CDC exposure management guidelines for varicella.
A surgical team is performing a liver transplant. Which of the following represents the HIGHEST risk for transmission of a healthcare-associated infection?
Options:
Failure to change surgical gloves after contamination.
Using alcohol-based hand rub instead of surgical scrub.
Delayed administration of preoperative antibiotics.
Airflow disruption due to personnel movement.
Answer:
AExplanation:
Glove Contamination and SSI Risk:
Failure to change contaminated gloves increases the risk of surgical site infections (SSIs).
Double-gloving with an outer glove change reduces contamination.
Why Other Options Are Incorrect:
B. Alcohol-based hand rubs: Are FDA-approved alternatives to traditional scrubs and effective.
C. Delayed antibiotics: Increases infection risk, but immediate correction reduces harm.
D. Airflow disruption: Can increase SSI risk, but glove contamination poses a more direct threat.
CBIC Infection Control References:
APIC-JCR Workbook, " Surgical Infection Prevention, " Chapter 6.
Which of the following anti-infective materials is used on endotracheal tubes, urine catheters, and intravascular catheters?
Options:
Silver
Copper
Chromium
Zinc
Answer:
AExplanation:
The CBIC Certified Infection Control Exam Study Guide (6th edition) identifies silver as an anti-infective material commonly incorporated into medical devices such as endotracheal tubes, urinary catheters, and intravascular catheters. Silver has broad-spectrum antimicrobial properties against bacteria, fungi, and some viruses. When used as a coating or impregnated material, silver ions disrupt microbial cell membranes, interfere with enzyme systems, and inhibit replication—thereby reducing microbial colonization and biofilm formation on device surfaces.
Device-associated infections often originate from colonization of indwelling devices. Silver-coated or silver-impregnated devices are intended to reduce the risk of healthcare-associated infections by limiting early microbial adherence and growth, particularly during the highest-risk period shortly after device insertion. Examples include silver alloy urinary catheters for CAUTI prevention and silver-coated endotracheal tubes designed to reduce ventilator-associated events.
The other options listed are not used in this context. Copper has antimicrobial properties but is not commonly used in indwelling medical devices. Chromium is used for corrosion resistance in alloys, not for infection prevention. Zinc plays roles in wound care and topical formulations but is not standard for catheter or tube coatings.
For CIC® exam preparation, recognizing silver as the anti-infective material used in multiple indwelling devices is important, as it reflects evidence-based strategies aimed at reducing device-associated infection risk.
==========
In the Preparedness and Response Framework for Influenza Pandemics, intervals are used to describe an influenza pandemic progression. The interval “Deceleration of the Pandemic Wave” is characterized by:
Options:
Subject matter experts’ judgment of the potential implications for human health.
Identification of novel influenza A in humans or animals anywhere in the world.
Low pandemic influenza activity but continued possible outbreaks.
Consistently decreasing rate of pandemic influenza cases.
Answer:
DExplanation:
The CBIC Certified Infection Control Exam Study Guide (6th edition) describes the Preparedness and Response Framework for Influenza Pandemics as a structured model that divides a pandemic into distinct intervals to guide public health and healthcare response activities. These intervals include investigation, recognition, initiation, acceleration, deceleration, and preparation for future waves.
The Deceleration of the Pandemic Wave interval is defined by a consistent and sustained decrease in the number of new pandemic influenza cases, hospitalizations, and deaths. This decline reflects the impact of mitigation strategies such as vaccination campaigns, antiviral use, nonpharmaceutical interventions, and the development of population immunity. Although transmission is decreasing, healthcare systems are advised to remain vigilant, as localized transmission may still occur.
Option A describes activities associated with the Investigation Interval, when experts assess the potential public health implications of a novel virus. Option B corresponds to the Recognition Interval, marked by identification of a novel influenza A virus. Option C aligns more closely with the Preparation for Future Waves Interval, when overall activity is low but the risk of resurgence remains.
Understanding these distinctions is critical for infection preventionists, as response priorities shift during each interval. During deceleration, focus transitions from surge response to recovery planning, evaluation of response effectiveness, and preparation for potential subsequent waves—key concepts emphasized in the CIC® exam.
==========
`
A microbiology laboratory plays a pivotal role in both endemic and epidemic epidemiology. Which of the following should be investigated FIRST?
Options:
One blood isolate of Streptococcus agalactiae in the nursery.
Two isolates of Staphylococcus aureus in postoperative surgical sites.
Three respiratory isolates of multi-drug resistant Klebsiella pneumoniae in the medical ICU.
Two blood isolates of coagulase-negative staphylococci in the oncology unit.
Answer:
CExplanation:
Multi-drug resistant (MDR) Klebsiella pneumoniae in a high-risk area like the ICU requires urgent investigation because:
It spreads rapidly via contaminated hands or equipment.
It poses a serious risk to immunocompromised patients.
An outbreak could lead to severe hospital-acquired infections (HAIs).
Why the Other Options Are Incorrect?
A. One blood isolate of Streptococcus agalactiae in the nursery – Single cases are not indicative of an outbreak.
B. Two isolates of Staphylococcus aureus in postoperative surgical sites – Common post-surgical pathogen; requires monitoring but not immediate outbreak investigation.
D. Two blood isolates of coagulase-negative staphylococci in the oncology unit – Common contaminants in blood cultures and not immediately alarming.
CBIC Infection Control Reference
APIC guidelines prioritize investigating MDR pathogens in high-risk units, such as ICU, to prevent transmission.
Why might identification of an infectious disease disaster related to bioterrorism or an outbreak of an emerging pathogen be difficult and/or delayed?
Options:
A novel strain of a pathogen could be involved.
The laboratory tests available for these pathogens have low sensitivity.
Over ten infected individuals/cases are needed before event identification can be confirmed.
Identification of bioterrorism attacks is done through blood donation surveillance, which is a slow process.
Answer:
AExplanation:
The CBIC Certified Infection Control Exam Study Guide (6th edition) explains that early identification of bioterrorism events or outbreaks caused by emerging pathogens is often challenging because a novel strain of a pathogen may be involved. Novel or emerging pathogens frequently present with nonspecific, influenza-like symptoms that resemble common community-acquired illnesses. As a result, early cases may not immediately raise concern among clinicians or public health authorities.
When a pathogen is novel, it may not be readily detectable using routine diagnostic tests, and clinicians may not initially consider it in their differential diagnosis. In addition, baseline epidemiologic patterns for the organism are often unknown, making it difficult to distinguish unusual disease activity from expected background illness. This delay can occur both in naturally emerging infections and in bioterrorism-related events where the organism or strain may be intentionally unfamiliar or genetically altered.
Option B is less accurate because the primary issue is often lack of recognition, not test sensitivity. Option C is incorrect because a specific number of cases is not required for detection; even a single unusual case can prompt investigation. Option D is incorrect because blood donation surveillance is not the primary mechanism for detecting bioterrorism or emerging infectious disease outbreaks.
For CIC® exam preparation, it is essential to recognize that novel pathogens obscure early recognition, delaying diagnosis, reporting, and response—making option A the most accurate answer.
The Infection Prevention and Control Committee is concerned about an outbreak of Serratia marcescens in the intensive care unit. If an environmental source is suspected, the BEST method to validate this suspicion is to
Options:
apply fluorescent gel.
use ATP system.
obtain surface cultures.
perform direct practice observation.
Answer:
CExplanation:
The correct answer is C, " obtain surface cultures, " as this is the best method to validate the suspicion of an environmental source for an outbreak of Serratia marcescens in the intensive care unit (ICU). According to the Certification Board of Infection Control and Epidemiology (CBIC) guidelines, Serratia marcescens is an opportunistic gram-negative bacterium commonly associated with healthcare-associated infections (HAIs), often linked to contaminated water, medical equipment, or environmental surfaces in ICUs. Obtaining surface cultures allows the infection preventionist (IP) to directly test environmental samples (e.g., from sinks, ventilators, or countertops) for the presence of Serratia marcescens, providing microbiological evidence to confirm or rule out an environmental source (CBIC Practice Analysis, 2022, Domain II: Surveillance and Epidemiologic Investigation, Competency 2.2 - Analyze surveillance data). This method is considered the gold standard for outbreak investigations when an environmental reservoir is suspected, as it offers specific pathogen identification and supports targeted interventions.
Option A (apply fluorescent gel) is a technique used to assess cleaning efficacy by highlighting areas missed during disinfection, but it does not directly identify the presence of Serratia marcescens or confirm an environmental source. Option B (use ATP system) measures adenosine triphosphate (ATP) to evaluate surface cleanliness and organic residue, which can indicate poor cleaning practices, but it is not specific to detecting Serratia marcescens and lacks the diagnostic precision of cultures. Option D (perform direct practice observation) is valuable for assessing staff adherence to infection control protocols, but it addresses human factors rather than directly validating an environmental source, making it less relevant as the initial step in this context.
The focus on obtaining surface cultures aligns with CBIC’s emphasis on using evidence-based methods to investigate and control HAIs, enabling the IP to collaborate with the committee to pinpoint the source and implement corrective measures (CBIC Practice Analysis, 2022, Domain II: Surveillance and Epidemiologic Investigation, Competency 2.3 - Identify risk factors for healthcare-associated infections). This approach is supported by CDC guidelines for outbreak investigations, which prioritize microbiological sampling to guide environmental control strategies (CDC Guidelines for Environmental Infection Control in Healthcare Facilities, 2019).
Which of the following statements describes the MOST important consideration of an infection preventionist when assessing the effectiveness of an infection control action plan?
Options:
Re-evaluate the action plan every three years.
Update the plan before the risk assessment is completed.
Develop a timeline and assign responsibilities for the stated action.
Monitor and validate the related outcome and process measures.
Answer:
DExplanation:
Assessing the effectiveness of an infection control action plan is a critical responsibility of an infection preventionist (IP) to ensure that interventions reduce healthcare-associated infections (HAIs) and improve patient safety. The Certification Board of Infection Control and Epidemiology (CBIC) highlights this process within the " Surveillance and Epidemiologic Investigation " and " Performance Improvement " domains, emphasizing the need for ongoing evaluation and data-driven decision-making. The Centers for Disease Control and Prevention (CDC) and other guidelines stress that the ultimate goal of an action plan is to achieve measurable outcomes, such as reduced infection rates, which requires systematic monitoring and validation.
Option D, " Monitor and validate the related outcome and process measures, " is the most important consideration. Outcome measures (e.g., infection rates, morbidity, or mortality) indicate whether the action plan has successfully reduced the targeted infection risk, while process measures (e.g., compliance with hand hygiene or proper catheter insertion techniques) assess whether the implemented actions are being performed correctly. Monitoring involves continuous data collection and analysis, while validation ensures the data’s accuracy and relevance to the plan’s objectives. The CBIC Practice Analysis (2022) underscores that effective infection control relies on evaluating both outcomes (e.g., decreased central line-associated bloodstream infections) and processes (e.g., adherence to aseptic protocols), making this a dynamic and essential step. The CDC’s " Compendium of Strategies to Prevent HAIs " (2016) further supports this by recommending regular surveillance and feedback as key to assessing intervention success.
Option A, " Re-evaluate the action plan every three years, " suggests a periodic review, which is a good practice for long-term planning but is insufficient as the most important consideration. Infection control requires more frequent assessment (e.g., quarterly or annually) to respond to emerging risks or outbreaks, making this less critical than ongoing monitoring. Option B, " Update the plan before the risk assessment is completed, " is illogical and counterproductive. Updating a plan without a completed risk assessment lacks evidence-based grounding, undermining the plan’s effectiveness and contradicting the CBIC’s emphasis on data-driven interventions. Option C, " Develop a timeline and assign responsibilities for the stated action, " is an important initial step in implementing an action plan, ensuring structure and accountability. However, it is a preparatory activity rather than the most critical factor in assessing effectiveness, which hinges on post-implementation evaluation.
The CBIC Practice Analysis (2022) and CDC guidelines prioritize outcome and process monitoring as the cornerstone of infection control effectiveness, enabling IPs to adjust strategies based on real-time evidence. Thus, Option D represents the most important consideration for assessing an infection control action plan’s success.
Which of the following management activities should be performed FIRST?
Options:
Evaluate project results
Establish goals
Plan and organize activities
Assign responsibility for projects
Answer:
BExplanation:
To determine which management activity should be performed first, we need to consider the logical sequence of steps in effective project or program management, particularly in the context of infection control as guided by CBIC principles. Management activities typically follow a structured process, and the order of these steps is critical to ensuring successful outcomes.
A. Evaluate project results: Evaluating project results involves assessing the outcomes and effectiveness of a project after its implementation. This step relies on having completed the project or at least reached a stage where outcomes can be measured. Performing this activity first would be premature, as there would be no results to evaluate without prior planning, goal-setting, and execution. Therefore, this cannot be the first step.
B. Establish goals: Establishing goals is the foundational step in any management process. Goals provide direction, define the purpose, and set the criteria for success. In the context of infection control, as emphasized by CBIC, setting clear objectives (e.g., reducing healthcare-associated infections by a specific percentage) is essential before any other activities can be planned or executed. This step aligns with the initial phase of strategic planning, making it the logical first activity. Without established goals, subsequent steps lack focus and purpose.
C. Plan and organize activities: Planning and organizing activities involve developing a roadmap to achieve the goals, including timelines, resources, and tasks. This step depends on having clear goals to guide the planning process. In infection control, this might include designing interventions to meet infection reduction targets. While critical, it cannot be the first step because planning requires a predefined objective to be effective.
D. Assign responsibility for projects: Assigning responsibility involves delegating tasks and roles to individuals or teams. This step follows the establishment of goals and planning, as responsibilities need to be aligned with the specific objectives and organized activities. In an infection control program, this might mean assigning staff to monitor compliance with hand hygiene protocols. Doing this first would be inefficient without a clear understanding of the goals and plan.
The correct sequence in management, especially in a structured field like infection control, begins with establishing goals to provide a clear target. This is followed by planning and organizing activities, assigning responsibilities, and finally evaluating results. The CBIC framework supports this approach by emphasizing the importance of setting measurable goals as part of the infection prevention and control planning process, which is a prerequisite for all subsequent actions.
CBIC Infection Prevention and Control (IPC) Core Competency Model (updated 2023), Domain V: Management and Communication, which highlights the importance of setting goals as the initial step in managing infection control programs.
CBIC Examination Content Outline, Domain V: Leadership and Program Management, which underscores the need for goal-setting prior to planning and implementation of infection control initiatives.
Over the past 6 months, a facility has noticed an increase in healthcare-associated pneumonias in ventilator-dependent patients in the NICU. There were eight healthcare-associated pneumonias among ventilated patients. Total ventilator days were 240. What was the ventilator-associated pneumonia rate for the NICU during the 6-month period?
Options:
33/1,000 ventilator days
30/1,000 ventilator days
3.3/1,000 ventilator days
3/1,000 ventilator days
Answer:
AExplanation:
The Certification Study Guide (6th edition) explains that device-associated infection rates are calculated using a standardized formula that expresses the number of infections per 1,000 device days. This allows comparison over time and between units with different patient volumes or device utilization.
The formula for ventilator-associated pneumonia (VAP) rate is:
(Number of VAPs ÷ Number of ventilator days) × 1,000
In this scenario, there were 8 ventilator-associated pneumonias and 240 ventilator days over the 6-month period.
8 ÷ 240 = 0.033
0.033 × 1,000 = 33.3 VAPs per 1,000 ventilator days
Rates are typically rounded to a whole number for reporting and benchmarking purposes, resulting in 33 per 1,000 ventilator days.
The study guide emphasizes that ventilator days—not patient days or admissions—are the correct denominator because they reflect time at risk for ventilator-associated infection. This approach ensures valid surveillance and supports accurate trend analysis and benchmarking.
The other answer choices represent incorrect calculations or decimal misplacement. Understanding rate calculations is a core CIC exam competency, particularly for interpreting device-associated infection data and guiding quality improvement initiatives in high-risk units such as NICUs.
==========
Which of the following processes would the catheter-associated urinary tract infection (CAUTI) improvement team choose as a process indicator to reduce CAUTI?
Options:
Documentation of indication for catheter placement
Rate of catheter-associated urinary tract infections
Reduction of catheter insertions per month
Rate of asymptomatic bacteriuria
Answer:
AExplanation:
A process indicator measures whether staff are reliably performing evidence-based practices that prevent infection (i.e., how well we do what we intend to do ). For CAUTI prevention, a core, guideline-supported strategy is to use indwelling urinary catheters only for appropriate indications and remove them as soon as they are no longer needed . Because inappropriate placement is a major driver of unnecessary catheter days (and therefore CAUTI risk), tracking whether the clinical indication is documented at insertion is a practical, auditable process measure that directly reflects adherence to appropriate-use policies. The CDC CAUTI prevention toolkit lists “compliance with documentation of catheter …” as an example of a process measure , aligning with performance measurement approaches recommended for CAUTI prevention.
In contrast, the CAUTI rate (option B) is an outcome measure , not a process measure. “Reduction of catheter insertions per month” (option C) reflects volume/usage trends rather than direct compliance with a specific practice, and “rate of asymptomatic bacteriuria” (option D) is not a recommended target metric for CAUTI prevention and routine screening for ASB is discouraged in CAUTI guidance.
A 2-yoar-old girl is admitted with a fractured tibia. At birth, she was diagnosed with congenital cytomegalovirus (CMV). Which of the following barrier precautions is appropriate for healthcare personnel caring for her?
Options:
Wear masks and gloves
Wear gloves when handling body fluids
No barrier precautions are needed
Use gowns, masks, gloves, and a private room
Answer:
BExplanation:
Standard Precautions are sufficient for congenital cytomegalovirus (CMV), which means that gloves should be used when handling body fluids. CMV is primarily transmitted via direct contact with saliva, urine, or blood.
Why the Other Options Are Incorrect?
A. Wear masks and gloves – Masks are not necessary unless performing high-risk aerosol-generating procedures.
C. No barrier precautions are needed – Gloves are required when handling bodily fluids to prevent transmission.
D. Use gowns, masks, gloves, and a private room – CMV does not require Contact or Airborne Precautions.
CBIC Infection Control Reference
APIC guidelines state that CMV transmission is prevented using Standard Precautions, primarily with glove use for body fluid contact.
A surgeon is beginning a new procedure in the facility within the next two weeks and requires loaner instruments. Infection prevention processes should ensure that
Options:
items arrive in time for immediate use steam sterilization.
instruments are able to be used prior to the biological indicator results.
the planning process takes place after the instruments have arrived.
staff education related to loaner instrument reprocessing has occurred.
Answer:
DExplanation:
The correct answer is D, " staff education related to loaner instrument reprocessing has occurred, " as this is the infection prevention process that should be ensured when a surgeon is beginning a new procedure requiring loaner instruments within the next two weeks. According to the Certification Board of Infection Control and Epidemiology (CBIC) guidelines, loaner instruments—those borrowed from external sources for temporary use—pose unique infection prevention challenges due to potential variability in reprocessing standards and unfamiliarity among staff. Ensuring that staff are educated on proper reprocessing protocols (e.g., cleaning, sterilization, and handling per manufacturer instructions and AAMI ST79) is critical to prevent healthcare-associated infections (HAIs) (CBIC Practice Analysis, 2022, Domain III: Infection Prevention and Control, Competency 3.3 - Ensure safe reprocessing of medical equipment). This education should cover the specific requirements for loaner instruments, including documentation and verification of sterilization, and should occur proactively before the instruments are used to ensure competency and compliance.
Option A (items arrive in time for immediate use steam sterilization) is a logistical consideration, but it does not address the infection prevention process itself; timely arrival is necessary but insufficient without proper reprocessing validation. Option B (instruments are able to be used prior to the biological indicator results) is unsafe, as biological indicators are essential to confirm sterilization efficacy, and using instruments before results are available violates infection control standards. Option C (the planning process takes place after the instruments have arrived) is impractical, as planning (e.g., coordinating with vendors, assessing reprocessing needs) must occur in advance to ensure readiness and safety, not as a reactive step.
The focus on staff education aligns with CBIC’s emphasis on preparing healthcare personnel to handle loaner instruments safely, reducing the risk of contamination and ensuring patient safety (CBIC Practice Analysis, 2022, Domain IV: Education and Research, Competency 4.1 - Develop and implement educational programs). This proactive measure is supported by AAMI and CDC guidelines, which stress the importance of training for reprocessing complex or unfamiliar devices.
When developing an exposure control plan, the MOST important aspect in the prevention of exposure to tuberculosis is:
Options:
Placement of the patient in an airborne infection isolation room.
Identification of a potentially infectious patient.
Prompt initiation of chemotherapeutic agents.
Use of personal protective equipment.
Answer:
BExplanation:
Tuberculosis (TB), caused by Mycobacterium tuberculosis, is an airborne disease that poses a significant risk in healthcare settings, particularly through exposure to infectious droplets. The Certification Board of Infection Control and Epidemiology (CBIC) emphasizes the " Prevention and Control of Infectious Diseases " domain, which includes developing exposure control plans, aligning with the Centers for Disease Control and Prevention (CDC) " Guidelines for Preventing the Transmission of Mycobacterium tuberculosis in Healthcare Settings " (2005). The question seeks the most important aspect of an exposure control plan to prevent TB exposure, requiring a prioritization of preventive strategies.
Option B, " Identification of a potentially infectious patient, " is the most important aspect. Early identification of individuals with suspected or confirmed TB (e.g., through symptom screening like persistent cough, fever, or weight loss, or diagnostic tests like chest X-rays and sputum smears) allows for timely isolation and treatment, preventing further transmission. The CDC guidelines stress that the first step in an exposure control plan is to recognize patients with signs or risk factors for infectious TB, as unrecognized cases are the primary source of healthcare worker and patient exposures. The Occupational Safety and Health Administration (OSHA) also mandates risk assessment and early detection as foundational to TB control plans.
Option A, " Placement of the patient in an airborne infection isolation room, " is a critical control measure once a potentially infectious patient is identified. Airborne infection isolation rooms (AIIRs) with negative pressure ventilation reduce the spread of infectious droplets, as recommended by the CDC. However, this step depends on prior identification; placing a patient in an AIIR without knowing their infectious status is inefficient and not the initial priority. Option C, " Prompt initiation of chemotherapeutic agents, " is essential for treating active TB and reducing infectiousness, typically within days of effective therapy, per CDC guidelines. However, this follows identification and diagnosis (e.g., via acid-fast bacilli smear or culture), making it a secondary action rather than the most important preventive aspect. Option D, " Use of personal protective equipment, " such as N95 respirators, is a key protective measure for healthcare workers once an infectious patient is identified, as outlined by the CDC and OSHA. However, PPE is a reactive measure that mitigates exposure after identification and isolation, not the foundational step to prevent it.
The CBIC Practice Analysis (2022) and CDC guidelines prioritize early identification as the cornerstone of TB exposure prevention, enabling all subsequent interventions. Option B ensures that the exposure control plan addresses the source of transmission at its outset, making it the most important aspect.
Education and training on safe work practices should be
Options:
Specific to a job or task.
Optional at the time of orientation.
Conducted in the nationally approved language.
Provided when policies and procedures are reviewed.
Answer:
AExplanation:
The CBIC Certified Infection Control Exam Study Guide (6th edition) emphasizes that education and training on safe work practices must be specific to the job or task performed. This principle aligns with occupational safety and infection prevention standards, which recognize that risks vary significantly depending on an employee’s role, responsibilities, and work environment. Training is most effective when it directly addresses the actual hazards staff may encounter and the specific procedures they are expected to perform.
Job- and task-specific training ensures that healthcare personnel understand how to apply safe practices in real-world situations, such as proper use of personal protective equipment, safe handling of sharps, device reprocessing, and exposure prevention. Generic or overly broad education may fail to address critical nuances and can result in gaps in compliance or increased risk of injury and infection.
Option B is incorrect because safety education is not optional and must be provided at orientation and ongoing as needed. Option C is misleading; while training should be provided in a language and format the employee understands, there is no concept of a single “nationally approved language.” Option D describes a possible timing for education but does not capture the core requirement that training be tailored to specific work activities.
For the CIC® exam, this question reinforces that effective infection prevention and occupational safety education must be job- and task-specific, making option A the correct answer.
An infection preventionist is utilizing the Shewhart/Deming cycle in an infection control program performance improvement project. In which of the following steps are the results of the interventions compared with the original goal?
Options:
Do
Act
Plan
Study
Answer:
DExplanation:
The correct answer is D, " Study, " as this is the step in the Shewhart/Deming cycle (commonly known as the Plan-Do-Study-Act [PDSA] cycle) where the results of the interventions are compared with the original goal. According to the Certification Board of Infection Control and Epidemiology (CBIC) guidelines, the PDSA cycle is a systematic approach to quality improvement, widely used in infection control programs to test and refine interventions. The cycle consists of four stages: Plan (designing the intervention and setting goals), Do (implementing the intervention on a small scale), Study (analyzing the data and comparing outcomes against the original goal), and Act (standardizing successful changes or adjusting based on findings) (CBIC Practice Analysis, 2022, Domain IV: Education and Research, Competency 4.2 - Evaluate the effectiveness of educational programs). The Study phase is critical for assessing whether the intervention achieved the intended reduction in infection rates or other performance metrics, providing evidence to guide the next steps.
Option A (Do) involves the execution of the planned intervention, focusing on implementation rather than evaluation, so it does not include comparing results. Option B (Act) is the final step where successful interventions are implemented on a broader scale or adjustments are made, but it follows the comparison made in the Study phase. Option C (Plan) is the initial stage of setting objectives and designing the intervention, which occurs before any results are available for comparison.
The emphasis on the Study phase aligns with CBIC’s focus on using data to evaluate the effectiveness of infection prevention strategies, ensuring that performance improvement projects are evidence-based and goal-oriented (CBIC Practice Analysis, 2022, Domain II: Surveillance and Epidemiologic Investigation, Competency 2.4 - Evaluate the effectiveness of infection prevention and control interventions). This step enables the infection preventionist to determine if the original goal—such as reducing healthcare-associated infections—was met, facilitating continuous improvement.
After defining and identifying cases in a possible cluster of infections, an infection preventionist should NEXT establish:
Options:
The route of transmission.
An appropriate control group.
A hypothesis that will explain the majority of cases.
Whether observed incidence exceeds expected incidence.
Answer:
CExplanation:
When investigating a possible cluster of infections, an infection preventionist (IP) follows a structured epidemiological approach to identify the cause and implement control measures. The Certification Board of Infection Control and Epidemiology (CBIC) outlines this process within the " Surveillance and Epidemiologic Investigation " domain, which aligns with the Centers for Disease Control and Prevention (CDC) guidelines for outbreak investigation. The steps typically include defining and identifying cases, formulating a hypothesis, testing the hypothesis, and implementing control measures. The question specifies the next step after defining and identifying cases, requiring an evaluation of the logical sequence.
Option C, " A hypothesis that will explain the majority of cases, " is the next critical step. After confirming a cluster through case definition and identification (e.g., by time, place, and person), the IP should develop a working hypothesis to explain the observed pattern. This hypothesis might propose a common source (e.g., contaminated equipment), a mode of transmission (e.g., airborne), or a specific population at risk. The CDC’s " Principles of Epidemiology in Public Health Practice " (3rd Edition, 2012) emphasizes that formulating a hypothesis is essential to guide further investigation, such as identifying risk factors or environmental sources. This step allows the IP to focus resources on testing the most plausible explanation before proceeding to detailed analysis or interventions.
Option A, " The route of transmission, " is an important element of the investigation but typically follows hypothesis formulation. Determining the route (e.g., contact, droplet, or common vehicle) requires data collection and analysis to test the hypothesis, making it a subsequent step rather than the immediate next action. Option B, " An appropriate control group, " is relevant for analytical studies (e.g., case-control studies) to compare exposed versus unexposed individuals, but this is part of hypothesis testing, which occurs after the hypothesis is established. Selecting a control group prematurely, without a hypothesis, lacks direction and efficiency. Option D, " Whether observed incidence exceeds expected incidence, " is a preliminary step to define a cluster, often done during case identification using baseline data or statistical thresholds (e.g., exceeding the mean plus two standard deviations). Since the question assumes cases are already defined and identified, this step is complete, and the focus shifts to hypothesis development.
The CBIC Practice Analysis (2022) and CDC guidelines prioritize hypothesis formulation as the logical next step after case identification, enabling a targeted investigation. This approach ensures that the IP can efficiently address the cluster’s cause, making Option C the correct answer.
The Sterile Processing Deportment alerts an infection preventionist that a load of surgical Instruments sterilized with high temperature steam:moist heat needs to be recalled. Which of the following Is the MOST likely reason for the recall?
Options:
Failure of the biological Indicator Bacillus subtilts
Failure of the biological Indicator Geobaciltus stearothermophilus
Placement of the biological Indicator on the bottom shelf over the d*an
Incorrect placement of the instruments In the tray
Answer:
BExplanation:
The most likely reason for the recall of a steam-sterilized load is the failure of the biological indicator (BI), specifically Geobacillus stearothermophilus, which is used to monitor high-temperature steam (moist heat) sterilization processes. This organism is the biological indicator of choice because it has high resistance to moist heat and thus serves as a reliable marker for sterilization efficacy.
The APIC Text and AAMI ST79 guidelines confirm that Geobacillus stearothermophilus is used for steam sterilization and that a failed BI indicates a failure in the sterilization process, which requires immediate action, including recalling all items sterilized since the last negative BI and reprocessing them. This is a crucial aspect of ensuring patient safety and preventing the use of potentially non-sterile surgical instruments.
According to the APIC Text:
" BIs are the only process indicators that directly monitor the lethality of a given sterilization process. [...] Geobacillus stearothermophilus spores are used to monitor steam sterilization... "
The CIC Study Guide (6th ed.) also specifies that:
" Evidence of sterilization failures (e.g., positive biological indicators) is the most common reason for a recall. "
Additionally, it is noted:
“With steam sterilization, the instrument load does not need to be recalled for a single positive biological indicator test, with the exception of implantable objects.”
However, multiple positive BIs or BI failure confirmation does require a recall.
The incorrect options explained:
A. Bacillus subtilis – This is not used in steam sterilization but rather in dry heat or EO processes.
C. Placement of the biological indicator on the bottom shelf over the drain – While incorrect placement can lead to test failure, the recall is prompted by BI failure, not just placement.
D. Incorrect placement of instruments – This can cause sterilization failure but is not the direct trigger for a recall unless it leads to a failed BI.
The cleaning and disinfection process that is appropriate for a particular surgical instrument depends on
Options:
all surgical instruments are cleaned and sterilized in the same manner.
instruments contaminated with blood must be bleach cleaned first.
the device manufacturer ' s written instructions for use.
the policies of the sterile processing department.
Answer:
CExplanation:
The correct answer is C, " the device manufacturer ' s written instructions for use, " as this is the factor that determines the appropriate cleaning and disinfection process for a particular surgical instrument. According to the Certification Board of Infection Control and Epidemiology (CBIC) guidelines, the reprocessing of surgical instruments must follow the specific instructions provided by the device manufacturer to ensure safety and efficacy. These instructions account for the instrument’s material, design, and intended use, specifying the appropriate cleaning agents, disinfection methods, sterilization techniques, and contact times to prevent damage and ensure the elimination of pathogens (CBIC Practice Analysis, 2022, Domain III: Infection Prevention and Control, Competency 3.3 - Ensure safe reprocessing of medical equipment). This is also mandated by regulatory standards, such as those from the Food and Drug Administration (FDA) and the Association for the Advancement of Medical Instrumentation (AAMI), which require adherence to manufacturer guidelines to maintain device integrity and patient safety.
Option A (all surgical instruments are cleaned and sterilized in the same manner) is incorrect because different instruments have unique characteristics (e.g., materials like stainless steel vs. delicate optics), necessitating tailored reprocessing methods rather than a one-size-fits-all approach. Option B (instruments contaminated with blood must be bleach cleaned first) is a misconception; while blood contamination requires thorough cleaning, bleach is not universally appropriate and may damage certain instruments unless specified by the manufacturer. Option D (the policies of the sterile processing department) may guide internal procedures but must be based on and subordinate to the manufacturer’s instructions to ensure compliance and effectiveness.
The emphasis on manufacturer instructions aligns with CBIC’s focus on evidence-based reprocessing practices to prevent healthcare-associated infections (HAIs) and protect patients (CBIC Practice Analysis, 2022, Domain III: Infection Prevention and Control, Competency 3.5 - Evaluate the environment for infection risks). Deviating from these guidelines can lead to inadequate sterilization or instrument damage, increasing infection risks.
A patient has a draining sinus at the site of a left total hip arthroplasty. A culture from the sinus tract reveals four organisms. Which of the following specimens is optimal for identifying the eliologic agent?
Options:
Blood
Wound drainage
Joint aspirate
Sinus tract tissue
Answer:
CExplanation:
The optimal specimen for identifying the etiologic agent in a prosthetic joint infection (PJI) is a joint aspirate (synovial fluid). This is because:
It provides direct access to the infected site without contamination from external sources.
It allows for accurate microbiologic culture, Gram stain, and leukocyte count analysis.
Why the Other Options Are Incorrect?
A. Blood – Blood cultures may help detect hematogenous spread but are not the best sample for identifying localized prosthetic joint infections.
B. Wound drainage – Wound cultures often contain contaminants from surrounding skin flora and do not accurately reflect joint space infection.
D. Sinus tract tissue – Cultures from sinus tracts often represent colonization rather than the primary infecting organism.
CBIC Infection Control Reference
APIC guidelines confirm that joint aspirate is the most reliable specimen for diagnosing prosthetic joint infections.
An infection preventionist (IP) is asked to assist in rewriting policies for insertion and maintenance of IV catheters. Which of the following are acceptable for use in site preparation?
Options:
Chloroxylenol or acetone
Povidone-iodine or para-chloro-meta-xylenol (PCMX)
Alcohol or chlorhexidine
Benzalkonium chloride or chlorhexidine
Answer:
CExplanation:
For IV catheter insertion, evidence-based guidance recommends preparing skin with an effective antiseptic agent to reduce skin flora at the insertion site and lower catheter-related infection risk. CDC guidance for prevention of intravascular catheter-related infections specifies that clean skin should be prepared with > 0.5% chlorhexidine (CHG) in alcohol for central venous catheter and peripheral arterial catheter insertion and during dressing changes. If CHG is contraindicated, CDC lists tincture of iodine, an iodophor, or 70% alcohol as acceptable alternatives.
Option C (Alcohol or chlorhexidine) is the only answer in which both agents are recognized as appropriate antiseptics for site preparation in intravascular catheter guidance (alcohol as an acceptable antiseptic option; CHG as preferred, typically in alcohol).
The other choices include agents that are not recommended as standard site-prep antiseptics for catheter insertion in major guidelines: acetone is not an antiseptic for vascular access site prep; benzalkonium chloride is generally considered less effective for this purpose compared with CHG/alcohol/iodophors; and PCMX/chloroxylenol is not the typical recommended agent for catheter insertion site antisepsis in these guidelines.
Surgical site infection (SSI) data for the previous quarter reveal the following numbers. The surgeon with the highest infection rate is Doctor
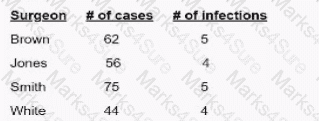
Options:
Brown
Jones.
Smith
White
Answer:
DExplanation:
To determine which surgeon has the highest surgical site infection (SSI) rate, use the following formula:
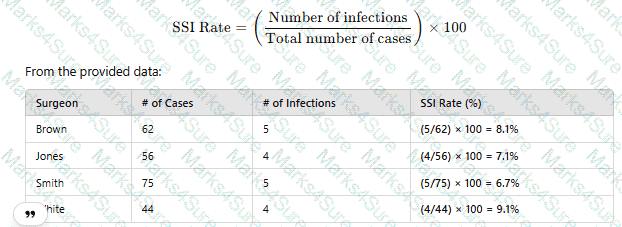
Since Dr. White has the highest SSI rate at 9.1%, the correct answer is D. White.
CBIC Infection Control Reference
SSI rates are calculated using infection count per total procedures and reported as percentage values.
An infection preventionist is informed that there is a possible cluster of streptococcal meningitis in the neonatal intensive care unit. Which of the following streptococcal serogroops is MOST commonly associated with meningitis in neonates beyond one week of age?
Options:
Group A
Group B
Group C
Group D
Answer:
BExplanation:
Group B Streptococcus (Streptococcus agalactiae) is the most common cause of neonatal bacterial meningitis beyond one week of age.
Step-by-Step Justification:
Group B Streptococcus (GBS) and Neonatal Infections:
GBS is a leading cause of late-onset neonatal meningitis (occurring after 7 days of age).
Infection typically occurs through vertical transmission from the mother or postnatal exposure.
Neonatal Risk Factors:
Premature birth, prolonged rupture of membranes, and maternal GBS colonization increase risk.
Why Other Options Are Incorrect:
A. Group A: Rare in neonates and more commonly associated with pharyngitis and skin infections.
C. Group C: Typically associated with animal infections and rarely affects humans.
D. Group D: Includes Enterococcus, which can cause neonatal infections but is not the most common cause of meningitis.
CBIC Infection Control References:
APIC Text, " Group B Streptococcus and Neonatal Meningitis " .
Which of the following factors is important in assessing the risk of Mycobacterium tuberculosis (MTB) exposure at a healthcare facility?
Options:
The number of cases of active MTB in the community served by the facility.
The number of airborne infection isolation rooms available within the facility.
The rate of healthcare personnel at the facility with positive MTB screening tests.
The compliance rate for annual N-95 fit testing among healthcare personnel at the facility.
Answer:
AExplanation:
The Certification Study Guide (6th edition) explains that assessment of Mycobacterium tuberculosis (MTB) risk in healthcare settings begins with evaluating the likelihood that patients with active TB will present to the facility. One of the most important determinants of this likelihood is the incidence of active TB disease in the community served by the healthcare facility. Facilities serving populations with higher TB prevalence are at increased risk of exposure events and must tailor their TB prevention and control programs accordingly.
The study guide emphasizes that TB risk assessments are population-based and epidemiologic in nature. Community TB rates directly influence the frequency with which undiagnosed or unsuspected infectious TB patients may enter the healthcare system, potentially exposing healthcare personnel (HCP) and other patients. This factor drives decisions regarding surveillance intensity, education, respiratory protection programs, and engineering controls.
The other options represent control measures or outcomes, not primary risk determinants. The number of airborne infection isolation rooms reflects facility preparedness, not exposure risk. Rates of positive HCP screening tests may indicate past exposure but are not used to assess initial risk. Compliance with N-95 fit testing is a program performance indicator, not a measure of TB exposure likelihood.
CIC exam questions commonly distinguish between risk assessment inputs versus mitigation strategies. Recognizing community TB incidence as the foundational risk factor is essential for accurate TB program planning and compliance with recommended infection prevention standards.
Which of the following findings indicates that a sputum sample has been properly collected from a patient with possible bacterial pneumonia?
Options:
Numerous neutrophils and few, if any, epithelial cells.
Presence of blood.
Many epithelial cells and few neutrophils.
Presence of both gram-positive and gram-negative bacteria.
Answer:
AExplanation:
The CBIC Certified Infection Control Exam Study Guide (6th edition) explains that the quality of a sputum specimen is critical for accurate diagnosis of bacterial pneumonia. A properly collected sputum sample should originate from the lower respiratory tract, not from saliva or the oropharynx. Microscopic examination of the specimen—typically using a Gram stain—is used to assess specimen adequacy before culture results are interpreted.
A high-quality sputum specimen is characterized by numerous neutrophils and few or no squamous epithelial cells. Neutrophils indicate an inflammatory response in the lower airways, consistent with bacterial infection. In contrast, epithelial cells originate from the mouth and upper respiratory tract; a large number of epithelial cells suggests contamination with saliva and an improperly collected specimen.
Option A correctly describes these criteria and therefore indicates proper specimen collection. Option C reflects poor-quality sputum contaminated with oral secretions and should be rejected or recollected. Option B (presence of blood) may occur in pneumonia but does not indicate specimen quality. Option D is nonspecific and may represent contamination or colonizing flora rather than true infection.
For the CIC® exam, it is important to recognize that specimen validity precedes interpretation of microbiologic results. The presence of abundant neutrophils with minimal epithelial cells confirms that the sputum sample is appropriate for diagnosing bacterial pneumonia and supports accurate clinical and epidemiologic decision-making.
The rate of catheter-associated urinary tract infections (CAUTIs) has decreased following recent practice changes. To present these results to the Quality Committee, the infection preventionist should use:
Options:
An affinity diagram.
A root cause analysis.
A run chart.
A fishbone diagram.
Answer:
CExplanation:
To communicate that CAUTI rates decreased after practice changes , the best tool is a run chart , which displays a measure over time and helps determine whether observed changes represent real improvement rather than random variation. The Institute for Healthcare Improvement (IHI) describes run charts as graphs of data over time and emphasizes that improvement and sustainability are demonstrated by observing patterns and shifts over time.
Run charts are especially appropriate for infection prevention metrics because they allow a Quality Committee to see: (1) the baseline period before interventions, (2) the timing of practice changes, and (3) whether there is a sustained downward trend or “shift” in CAUTI rates. Patient safety measurement guidance likewise notes that run charts are a standard quality tool to display trends in patient-safety measures over time and evaluate whether process changes are leading to improvement.
By contrast, an affinity diagram organizes ideas/themes, and fishbone diagrams and root cause analyses are primarily for analyzing causes of a problem—not for clearly presenting a time-based improvement result to leadership. A run chart is therefore the most appropriate communication method.
A review of bronchoscopy specimens indicates an unusual number of Mycobacterium fortuitum–positive cultures. Which of the following observations would be the MOST likely cause of this finding?
Options:
Bronchoscopes cleaned with sporicidal solution
Inadequate cleaning prior to disinfection
Rinsing with tap water
Drying with air or alcohol
Answer:
CExplanation:
The CBIC Certified Infection Control Exam Study Guide (6th edition) identifies nontuberculous mycobacteria (NTM), including Mycobacterium fortuitum, as organisms commonly associated with water sources, particularly potable water systems. An unusual increase in M. fortuitum–positive bronchoscopy cultures is most often linked to waterborne contamination during endoscope reprocessing, making rinsing with tap water the most likely cause.
Tap water is not sterile and may harbor NTM, which are resistant to standard municipal water treatment and capable of forming biofilms within plumbing systems. If bronchoscopes are rinsed with tap water after high-level disinfection and not followed by appropriate sterile or filtered water rinses and thorough drying, organisms such as M. fortuitum may contaminate internal channels. This can lead to pseudo-outbreaks, where cultures are positive due to contamination rather than true patient infection.
Option B, inadequate cleaning prior to disinfection, can contribute to overall reprocessing failure but is less specifically associated with NTM contamination patterns. Option A is unlikely, as sporicidal solutions are effective disinfectants. Option D, drying with air or alcohol, is a recommended step to reduce microbial growth and would not cause contamination.
For CIC® exam preparation, recognizing that tap water exposure during endoscope reprocessing is a classic source of nontuberculous mycobacteria contamination is a key concept in outbreak investigation and device reprocessing surveillance.
A team was created to determine what has contributed to the recent increase in catheter associated urinary tract infections (CAUTIs). What quality tool should the team use?
Options:
Gap analysis
Fishbone diagram
Plan, do, study, act (PDSA)
Failure mode and effect analysis (FMEA)
Answer:
BExplanation:
The correct answer is B, " Fishbone diagram, " as this is the most appropriate quality tool for the team to use when determining what has contributed to the recent increase in catheter-associated urinary tract infections (CAUTIs). According to the Certification Board of Infection Control and Epidemiology (CBIC) guidelines, the fishbone diagram, also known as an Ishikawa or cause-and-effect diagram, is a structured tool used to identify and categorize potential causes of a problem. In this case, the team needs to explore the root causes of the CAUTI increase, which could include factors such as improper catheter insertion techniques, inadequate maintenance, staff training gaps, or environmental issues (CBIC Practice Analysis, 2022, Domain II: Surveillance and Epidemiologic Investigation, Competency 2.2 - Analyze surveillance data). The fishbone diagram organizes these causes into categories (e.g., people, process, equipment, environment), facilitating a comprehensive analysis and guiding further investigation or intervention.
Option A (gap analysis) is useful for comparing current performance against a desired standard or benchmark, but it is more suited for identifying deficiencies in existing processes rather than uncovering the specific causes of a recent increase. Option C (plan, do, study, act [PDSA]) is a cyclical quality improvement methodology for testing and implementing changes, which would be relevant after identifying causes and designing interventions, not as the initial tool for root cause analysis. Option D (failure mode and effect analysis [FMEA] ) is a proactive risk assessment tool used to predict and mitigate potential failures in a process before they occur, making it less applicable to analyzing an existing increase in CAUTIs.
The use of a fishbone diagram aligns with CBIC’s emphasis on using data-driven tools to investigate and address healthcare-associated infections (HAIs) like CAUTIs, supporting the team’s goal of pinpointing contributory factors (CBIC Practice Analysis, 2022, Domain II: Surveillance and Epidemiologic Investigation, Competency 2.3 - Identify risk factors for healthcare-associated infections). This tool’s visual and collaborative nature also fosters team engagement, which is essential for effective problem-solving in infection prevention.
Which of the following is the correct collection technique to obtain a laboratory specimen for suspected pertussis?
Options:
Cough plate
Nares culture
Sputum culture
Nasopharyngeal culture
Answer:
DExplanation:
The gold standard specimen for diagnosing pertussis (Bordetella pertussis infection) is a nasopharyngeal culture because:
B. pertussis colonizes the nasopharynx, making it the best site for detection.
A properly collected nasopharyngeal swab or aspirate increases diagnostic sensitivity.
This method is recommended for culture, PCR, or direct fluorescent antibody testing.
Why the Other Options Are Incorrect?
A. Cough plate – Not commonly used due to low sensitivity.
B. Nares culture – The nares are not a primary site for pertussis colonization.
C. Sputum culture – B. pertussis does not commonly infect the lower respiratory tract.
CBIC Infection Control Reference
APIC confirms that nasopharyngeal culture is the preferred method for diagnosing pertussis.
Which of the following factors should be considered when evaluating countertop surface materials?
Options:
Durability
Sink design
Accessibility
Faucet placement
Answer:
AExplanation:
The correct answer is A, " Durability, " as it is a critical factor to consider when evaluating countertop surface materials. According to the Certification Board of Infection Control and Epidemiology (CBIC) guidelines, the selection of materials in healthcare settings, including countertop surfaces, must prioritize infection prevention and control. Durability ensures that the surface can withstand frequent cleaning, disinfection, and physical wear without degrading, which is essential to maintain a hygienic environment and prevent the harboring of pathogens (CBIC Practice Analysis, 2022, Domain III: Infection Prevention and Control, Competency 3.4 - Implement environmental cleaning and disinfection protocols). Durable materials, such as solid surface composites or stainless steel, resist scratches, cracks, and moisture damage, reducing the risk of microbial growth and cross-contamination, which are significant concerns in healthcare facilities.
Option B (sink design) relates more to the plumbing and fixture layout rather than the inherent properties of the countertop material itself. While sink placement and design are important for workflow and hygiene, they are secondary to the material ' s characteristics. Option C (accessibility) is a consideration for user convenience and compliance with the Americans with Disabilities Act (ADA), but it pertains more to the installation and layout rather than the material ' s suitability for infection control. Option D (faucet placement) affects usability and water management but is not a direct attribute of the countertop material.
The emphasis on durability aligns with CBIC’s focus on creating environments that support effective cleaning and disinfection practices, which are vital for preventing healthcare-associated infections (HAIs). Selecting durable materials helps ensure long-term infection prevention efficacy, making it a primary factor in the evaluation process (CBIC Practice Analysis, 2022, Domain III: Infection Prevention and Control, Competency 3.5 - Evaluate the environment for infection risks).
An infection preventionist (IP) notices that several discharged newborns have been readmitted with staphylococcal infections. What should the IP do FIRST?
Options:
Observe medical and nursing techniques in the nursery.
Obtain surveillance cultures on babies in the nursery.
Begin prospective surveillance to identify new staphylococcal cases.
Review medical records of the readmitted cases.
Answer:
DExplanation:
The Certification Study Guide (6th edition) outlines a structured approach to outbreak investigation, emphasizing that the first step is to verify the problem and establish baseline facts before initiating control measures. When an infection preventionist becomes aware of potential clustering—such as multiple newborn readmissions with staphylococcal infections—the initial priority is to review the medical records of the affected cases.
Reviewing records allows the IP to confirm diagnoses, identify common organisms, determine timing of symptom onset, and assess potential epidemiologic links (e.g., same nursery, staff exposure, procedures, or length of stay). This step helps determine whether the cases represent a true outbreak, coincidental community-acquired infections, or unrelated events. The study guide stresses that interventions should not begin until the problem is clearly defined, as premature actions may waste resources or obscure the true source.
The other options are appropriate later steps in an investigation. Observing practices and obtaining surveillance cultures are targeted control measures that should follow confirmation of an outbreak and hypothesis generation. Beginning prospective surveillance is also important, but only after case definitions and baseline data are established.
CIC exam questions frequently test sequencing of outbreak investigation steps. Recognizing that case confirmation and record review come first is essential for effective infection prevention decision-making and accurate epidemiologic analysis.
In an outbreak of probable foodborne illness, a group of individuals develops watery diarrhea 48 hours after eating imported shellfish. The MOST likely causative organism is:
Options:
Vibrio cholerae
Hepatitis A virus
Staphylococcus aureus
Listeria monocytogenes
Answer:
AExplanation:
The CBIC Certified Infection Control Exam Study Guide (6th edition) highlights that consumption of raw or undercooked shellfish, particularly imported shellfish, is a well-recognized risk factor for waterborne and foodborne Vibrio infections, including Vibrio cholerae. The organism thrives in warm coastal waters and can contaminate shellfish harvested from endemic or inadequately regulated regions.
The clinical presentation described—profuse watery diarrhea occurring approximately 48 hours after exposure—is classic for Vibrio cholerae. The organism produces cholera toxin, which causes rapid fluid secretion into the intestinal lumen, resulting in large-volume watery stools. The incubation period typically ranges from a few hours to five days, making a 48-hour onset highly consistent with this pathogen.
The other options are less likely based on incubation period and symptom profile. Hepatitis A virus has an incubation period of weeks and presents with jaundice rather than acute watery diarrhea. Staphylococcus aureus food poisoning causes rapid onset (1–6 hours) due to preformed toxin and is commonly associated with vomiting. Listeria monocytogenes typically causes invasive disease rather than acute watery diarrhea and has a longer incubation period.
For CIC® exam preparation, recognizing shellfish-associated watery diarrhea with short incubation as characteristic of Vibrio cholerae is essential, particularly in outbreak investigations involving imported seafood.
Which of the following is an example of an outcome measure?
Options:
Hand hygiene compliance rate
Adherence to Environmental Cleaning
Rate of multi-drug resistant organisms acquisition
Timing of preoperative antibiotic administration
Answer:
CExplanation:
The correct answer is C, " Rate of multi-drug resistant organisms acquisition, " as it represents an example of an outcome measure. According to the Certification Board of Infection Control and Epidemiology (CBIC) guidelines, outcome measures are indicators that reflect the impact or result of infection prevention and control interventions on patient health outcomes or the incidence of healthcare-associated infections (HAIs). The rate of multi-drug resistant organisms (MDRO) acquisition directly measures the incidence of new infections caused by resistant pathogens, which is a key outcome affected by the effectiveness of infection control practices (CBIC Practice Analysis, 2022, Domain II: Surveillance and Epidemiologic Investigation, Competency 2.4 - Evaluate the effectiveness of infection prevention and control interventions).
Option A (hand hygiene compliance rate) is an example of a process measure, which tracks adherence to specific protocols or practices intended to prevent infections, rather than the resulting health outcome. Option B (adherence to environmental cleaning) is also a process measure, focusing on the implementation of cleaning protocols rather than the end result, such as reduced infection rates. Option D (timing of preoperative antibiotic administration) is another process measure, assessing the timeliness of an intervention to prevent surgical site infections, but it does not directly indicate the outcome (e.g., infection rate) of that intervention.
Outcome measures, such as the rate of MDRO acquisition, are critical for evaluating the success of infection prevention programs and are often used to guide quality improvement initiatives. This aligns with CBIC’s emphasis on using surveillance data to assess the effectiveness of interventions and inform decision-making (CBIC Practice Analysis, 2022, Domain II: Surveillance and Epidemiologic Investigation, Competency 2.5 - Use data to guide infection prevention and control strategies). The focus on MDRO acquisition specifically highlights a significant healthcare challenge, making it a prioritized outcome measure in infection control.
An infection preventionist is calculating measures of central tendency regarding duration of a surgical procedure using this data set: 2, 2, 3, 4, and 9. Which of the following statements is correct?
Options:
The median is 2.
The mode is 3.
The mean is 4.
The standard deviation is 7.
Answer:
CExplanation:
Measures of central tendency (mean, median, mode) and dispersion (standard deviation) are statistical tools used to summarize data, such as the duration of surgical procedures, which can help infection preventionists identify trends or risks for surgical site infections. The Certification Board of Infection Control and Epidemiology (CBIC) supports the use of data analysis in the " Surveillance and Epidemiologic Investigation " domain, aligning with epidemiological principles outlined by the Centers for Disease Control and Prevention (CDC). The question provides a data set of 2, 2, 3, 4, and 9, and requires determining the correct statement by calculating these measures.
Mean: The mean is the average of the data set, calculated by summing all values and dividing by the number of observations. For the data set 2, 2, 3, 4, and 9:(2 + 2 + 3 + 4 + 9) ÷ 5 = 20 ÷ 5 = 4. Thus, the mean is 4, making Option C correct.
Median: The median is the middle value when the data set is ordered. With five values (2, 2, 3, 4, 9), the middle value is the third number, which is 3. Option A states the median is 2, which is incorrect.
Mode: The mode is the most frequently occurring value. In this data set, 2 appears twice, while 3, 4, and 9 appear once each, making 2 the mode. Option B states the mode is 3, which is incorrect.
Standard Deviation: The standard deviation measures the spread of data around the mean. For a small data set like this, the calculation involves finding the variance (average of squared differences from the mean) and taking the square root. The mean is 4, so the deviations are: (2-4)² = 4, (2-4)² = 4, (3-4)² = 1, (4-4)² = 0, (9-4)² = 25. The sum of squared deviations is 4 + 4 + 1 + 0 + 25 = 34. The variance is 34 ÷ 5 = 6.8, and the standard deviation is √6.8 ≈ 2.61 (not 7). Option D states the standard deviation is 7, which is incorrect without further context (e.g., a population standard deviation with n-1 denominator would be √34 ≈ 5.83, still not 7).
The CBIC Practice Analysis (2022) and CDC guidelines encourage accurate statistical analysis to inform infection control decisions, such as assessing surgical duration as a risk factor for infections. Based on the calculations, the mean of 4 is the only correct statement among the options, confirming Option C as the answer. Note that the standard deviation of 7 might reflect a miscalculation or misinterpretation (e.g., using a different formula or data set), but with the given data, it does not hold.
Some pathogens live in the body and can be cultured, but do NOT elicit any response from the body’s defense mechanisms. This state is called:
Options:
Colonization
Infection
Latency
Contamination
Answer:
AExplanation:
The interaction between pathogens and the human body can take various forms, each with distinct immunological and clinical implications. The Certification Board of Infection Control and Epidemiology (CBIC) emphasizes understanding these states within the " Identification of Infectious Disease Processes " domain to guide infection prevention strategies. The question describes a scenario where pathogens are present, can be cultured (indicating viable organisms), but do not trigger a response from the body’s defense mechanisms, such as inflammation or immune activation. This requires identifying the appropriate microbiological state.
Option A, " Colonization, " is the correct answer. Colonization occurs when microorganisms are present on or in the body (e.g., skin, mucous membranes, or gut) without causing harm or eliciting an immune response. These pathogens can be cultured, as they are alive and replicating, but they exist in a commensal or symbiotic relationship with the host, not provoking symptoms or defense mechanisms. Examples include normal flora like Staphylococcus epidermidis on the skin or Streptococcus salivarius in the oral cavity. The Centers for Disease Control and Prevention (CDC) defines colonization as the presence of microbes without tissue invasion or damage, distinguishing it from infection (CDC, " Principles of Epidemiology in Public Health Practice, " 3rd Edition, 2012).
Option B, " Infection, " is incorrect because it involves the invasion and multiplication of pathogens in body tissues, leading to an immune response, such as inflammation, fever, or antibody production. This contrasts with the question’s description of no defense mechanism response. Option C, " Latency, " refers to a state where a pathogen (e.g., herpes simplex virus or Mycobacterium tuberculosis) remains dormant in the body after initial infection, capable of reactivation but not eliciting an active immune response during dormancy. However, latency implies a prior infection with a latent phase, whereas the question suggests a current, non-responsive state without prior infection context. Option D, " Contamination, " describes the unintended presence of pathogens on inanimate objects or surfaces (e.g., medical equipment), not within the body, and does not align with the scenario of living, culturable pathogens in a host.
The CBIC Practice Analysis (2022) and CDC guidelines highlight colonization as a key concept in infection control, particularly in settings like hospitals where colonized patients can serve as reservoirs for potential infections. The absence of an immune response, as specified, aligns with the definition of colonization, making Option A the most accurate answer.
An infection preventionist (IP) reviews research from a current publication and compares the data to the IP’s facility data. This is an example of:
Options:
Benchmarking
Data collection
Linear regression
Data mining
Answer:
AExplanation:
The Certification Study Guide (6th edition) defines benchmarking as the process of comparing an organization’s performance data with external reference points, such as published research, national databases, or peer institutions. In this scenario, the infection preventionist is comparing the facility’s data to findings from a current publication, which clearly represents benchmarking activity.
Benchmarking allows infection preventionists to determine how their facility is performing relative to recognized standards, evidence-based outcomes, or peer performance. The study guide emphasizes that benchmarking is essential for identifying performance gaps, prioritizing improvement initiatives, and supporting data-driven decision-making. It is frequently used when evaluating infection rates, compliance metrics, and outcomes associated with prevention strategies.
The other options do not accurately describe this activity. Data collection refers to the gathering of raw data, not comparison. Linear regression is a statistical analysis method used to examine relationships between variables over time and is not implied in this scenario. Data mining involves exploring large datasets to identify patterns or associations, typically without a predefined comparison target.
CIC exam questions often test understanding of data use versus data analysis methods. Recognizing benchmarking as the comparison of internal performance to external standards is a foundational competency for infection preventionists. This practice supports quality improvement, regulatory compliance, and leadership reporting.
A family, including an infant of 8 months, is going on a vacation to Europe. An infection preventionist would recommend:
Options:
Exposure to rabies should be avoided.
Family members should be vaccinated for yellow fever.
The infant should not travel until at least 12 months of age.
Family immunization records should be reviewed by their provider.
Answer:
DExplanation:
When advising a family, including an 8-month-old infant, planning a vacation to Europe, an infection preventionist (IP) must consider travel-related health risks and vaccination recommendations tailored to the destination and age-specific guidelines. The Certification Board of Infection Control and Epidemiology (CBIC) emphasizes the " Education and Training " domain, which includes providing evidence-based advice to prevent infections, aligning with the Centers for Disease Control and Prevention (CDC) and World Health Organization (WHO) travel health recommendations.
Option D, " Family immunization records should be reviewed by their provider, " is the most appropriate recommendation. Europe, as a region, includes countries with varying health risks, but it is generally considered a low-risk area for many vaccine-preventable diseases compared to tropical regions. The CDC’s " Travelers’ Health " guidelines (2023) recommend that all travelers, including infants, have their immunization status reviewed by a healthcare provider prior to travel to ensure compliance with routine vaccinations (e.g., measles, mumps, rubella [MMR], diphtheria, tetanus, pertussis [DTaP] , and polio) and to assess any destination-specific needs. For an 8-month-old, the review would confirm that the infant has received age-appropriate vaccines (e.g., the first doses of DTaP, Hib, PCV, and IPV, typically starting at 2 months) and is on schedule for the 6- and 12-month doses. This step ensures the family’s overall protection and identifies any gaps, making it a proactive and universally applicable recommendation.
Option A, " Exposure to rabies should be avoided, " is a general travel safety tip applicable to any destination where rabies is endemic (e.g., parts of Eastern Europe or rural areas with wildlife). However, rabies risk in most European countries is low, and pre-exposure vaccination is not routinely recommended for travelers unless specific high-risk activities (e.g., handling bats) are planned. The CDC advises avoiding animal bites rather than vaccinating unless indicated, making this less specific and urgent than a records review. Option B, " Family members should be vaccinated for yellow fever, " is incorrect. Yellow fever is not endemic in Europe, and vaccination is not required or recommended for travel to any European country. The WHO International Health Regulations (2005) and CDC list yellow fever vaccination as mandatory only for travelers from or to certain African and South American regions, rendering this irrelevant. Option C, " The infant should not travel until at least 12 months of age, " lacks a clear evidence base. While some vaccines (e.g., MMR) are typically given at 12 months, the 8-month-old can travel safely if up-to-date on age-appropriate immunizations. The CDC allows travel for infants as young as 6 weeks with medical clearance, and delaying travel to 12 months is not a standard recommendation unless specific risks (e.g., disease outbreaks) are present, which are not indicated here.
The CBIC Practice Analysis (2022) and CDC Travelers’ Health resources prioritize pre-travel health assessments, including immunization reviews, as the foundation for safe travel. Option D ensures a comprehensive approach tailored to the family’s needs, making it the best recommendation for a trip to Europe.
Which of the following should be included when designing a data collection form for surveillance?
Options:
Denominator information
Only the information needed
As much information as possible
Medication history
Answer:
AExplanation:
The Certification Study Guide (6th edition) emphasizes that effective surveillance depends on the ability to calculate rates, not just counts. To calculate any infection rate, both a numerator (number of infection events) and a denominator (population at risk or time at risk) are required. Therefore, inclusion of denominator information is essential when designing a data collection form for surveillance.
Denominator data may include patient days, device days (e.g., central line days, ventilator days), number of procedures, or number of admissions—depending on the surveillance objective. Without denominator data, infection preventionists cannot calculate standardized rates, compare trends over time, or benchmark against national databases. The study guide clearly states that surveillance systems lacking denominator data produce incomplete and potentially misleading results.
The other options are either vague or inappropriate. While data collection forms should avoid unnecessary information, simply stating “only the information needed” does not address the critical requirement for denominator data. Collecting “as much information as possible” is discouraged because it increases workload, reduces data quality, and may compromise sustainability of surveillance programs. Medication history is not routinely required for most surveillance activities unless it is directly related to the infection being studied.
This question reflects a fundamental CIC exam principle: surveillance must be designed to support valid rate calculation and analysis. Including denominator information ensures that collected data are meaningful, actionable, and aligned with evidence-based infection prevention practices.
Following an outbreak of Hepatitis A, the water supply is sampled. A high count of which of the following isolates would indicate that the water was a potential source?
Options:
Coliforms
Pseudomonads
Legionella
Acinetobacter
Answer:
AExplanation:
Coliform bacteria are indicators of fecal contamination in water, making them a critical measure of water safety. Hepatitis A is a virus primarily transmitted via the fecal-oral route, often through contaminated food or water.
Step-by-Step Justification:
Fecal Contamination and Hepatitis A:
Hepatitis A virus (HAV) spreads through ingestion of water contaminated with fecal matter. High coliform counts indicate fecal contamination and increase the risk of HAV outbreaks.
Use of Coliforms as Indicators:
Public health agencies use total coliforms and Escherichia coli (E. coli) as primary indicators of water safety because they signal fecal pollution.
Waterborne Transmission of Hepatitis A:
Hepatitis A outbreaks have been traced to contaminated drinking water, ice, and improperly treated wastewater. Coliform detection signals a need for immediate action.
Why Other Options Are Incorrect:
B. Pseudomonads:
Pseudomonads (e.g., Pseudomonas aeruginosa) are environmental bacteria but are not indicators of fecal contamination.
C. Legionella:
Legionella species cause Legionnaires ' disease through inhalation of contaminated aerosols, not through fecal-oral transmission.
D. Acinetobacter:
Acinetobacter species are opportunistic pathogens in healthcare settings but are not indicators of waterborne fecal contamination.
CBIC Infection Control References:
APIC Text, " Water Systems and Infection Control Measures " .
APIC Text, " Hepatitis A Transmission and Waterborne Outbreaks " .
The infection preventionist (IP) is working with the Product Evaluation Committee to select a sporicidal disinfectant for Clostridioides difficile. An effective disinfectant for the IP to recommend is
Options:
quaternary ammonium compound.
phenolic.
isopropyl alcohol.
sodium hypochlorite.
Answer:
DExplanation:
The correct answer is D, " sodium hypochlorite, " as it is an effective sporicidal disinfectant for Clostridioides difficile that the infection preventionist (IP) should recommend. According to the Certification Board of Infection Control and Epidemiology (CBIC) guidelines, Clostridioides difficile (C. difficile) is a spore-forming bacterium responsible for significant healthcare-associated infections (HAIs), and its spores are highly resistant to many common disinfectants. Sodium hypochlorite (bleach) is recognized by the Centers for Disease Control and Prevention (CDC) and the Environmental Protection Agency (EPA) as a sporicidal agent capable of inactivating C. difficile spores when used at appropriate concentrations (e.g., 1:10 dilution of household bleach) and with the recommended contact time (CBIC Practice Analysis, 2022, Domain III: Infection Prevention and Control, Competency 3.4 - Implement environmental cleaning and disinfection protocols). This makes it a preferred choice for environmental disinfection in outbreak settings or areas with known C. difficile contamination.
Option A (quaternary ammonium compound) is effective against many bacteria and viruses but lacks sufficient sporicidal activity against C. difficile spores, rendering it inadequate for this purpose. Option B (phenolic) has broad-spectrum antimicrobial properties but is not reliably sporicidal and is less effective against C. difficile spores compared to sodium hypochlorite. Option C (isopropyl alcohol) is useful for disinfecting surfaces and killing some pathogens, but it is not sporicidal and evaporates quickly, making it ineffective against C. difficile spores.
The IP’s recommendation of sodium hypochlorite aligns with CBIC’s emphasis on selecting disinfectants based on their efficacy against specific pathogens and adherence to evidence-based guidelines (CBIC Practice Analysis, 2022, Domain III: Infection Prevention and Control, Competency 3.5 - Evaluate the environment for infection risks). Proper use, including correct dilution and contact time, is critical to ensure effectiveness, and the IP should collaborate with the Product Evaluation Committee to ensure implementation aligns with safety and regulatory standards (CDC Guidelines for Environmental Infection Control in Healthcare Facilities, 2019).
An infection preventionist reviewing patient records in an outpatient hemodialysis center notes an increase in localized infections at catheter access sites. Which of the following strategies reduces the risk of infection in this population?
Options:
Creation of an arteriovenous fistula
Use of a non-cuffed percutaneous catheter
Placement of a femoral catheter
Replacement of dialysis catheters monthly
Answer:
AExplanation:
The best strategy to reduce the risk of infection in hemodialysis patients is to use an arteriovenous (AV) fistula as the preferred vascular access method. AV fistulas have the lowest infection rates compared to catheters and grafts because they do not involve foreign material and are less prone to biofilm formation and bloodstream infections.
Why the Other Options Are Incorrect?
B. Use of a non-cuffed percutaneous catheter – Non-cuffed catheters have a higher risk of bloodstream infections and should be used only for short-term access.
C. Placement of a femoral catheter – Femoral catheters have higher infection risks and should only be used for bed-bound patients and for the shortest duration possible.
D. Replacement of dialysis catheters monthly – Routine catheter replacement does not reduce infection risk and should be done only when medically necessary.
CBIC Infection Control Reference
According to APIC guidelines, AV fistulas are the preferred vascular access due to their lower infection rates and improved long-term outcomes.
The Environmental Services department is purchasing a new disinfectant that is an approved hospital disinfectant with no tuberculocidal claim. This product is appropriate for cleaning which of the following items?
Options:
Laryngoscope blades
Blood pressure cuff
Respiratory therapy equipment
Ultrasound probe
Answer:
BOn January 31, the nursing staff of a long-term care facility reports that five out of 35 residents have developed high fever, nasal discharge, and a dry cough. The BEST diagnostic tool to determine the causative agent is:
Options:
Blood culture
Sputum culture
Nasopharyngeal swab
Legionella serology
Answer:
CExplanation:
The scenario describes a cluster of five out of 35 residents in a long-term care facility developing high fever, nasal discharge, and a dry cough, suggesting a potential respiratory infection outbreak. The Certification Board of Infection Control and Epidemiology (CBIC) emphasizes the " Identification of Infectious Disease Processes " and " Surveillance and Epidemiologic Investigation " domains, which require selecting the most appropriate diagnostic tool to identify the causative agent promptly. The Centers for Disease Control and Prevention (CDC) provides guidance on diagnostic approaches for respiratory infections, particularly in congregate settings like long-term care facilities.
Option C, " Nasopharyngeal swab, " is the best diagnostic tool in this context. The symptoms—high fever, nasal discharge, and a dry cough—are characteristic of upper respiratory infections, such as influenza, respiratory syncytial virus (RSV), or other viral pathogens common in congregate settings. A nasopharyngeal swab is the gold standard for detecting these agents, as it collects samples from the nasopharynx, where many respiratory viruses replicate. The CDC recommends nasopharyngeal swabs for molecular testing (e.g., PCR) to identify viruses like influenza, RSV, or SARS-CoV-2, especially during outbreak investigations in healthcare facilities. The dry cough and nasal discharge align with upper respiratory involvement, making this sample type more targeted than alternatives. Given the potential for rapid spread among vulnerable residents, early identification via nasopharyngeal swab is critical to guide infection control measures.
Option A, " Blood culture, " is less appropriate as the best initial tool. Blood cultures are used to detect systemic bacterial infections (e.g., bacteremia or sepsis), but the symptoms described are more suggestive of a primary respiratory infection rather than a bloodstream infection. While secondary bacteremia could occur, blood cultures are not the first-line diagnostic for this presentation and are more relevant if systemic signs (e.g., hypotension) worsen. Option B, " Sputum culture, " is useful for lower respiratory infections, such as pneumonia, where productive cough and sputum production are prominent. However, the dry cough and nasal discharge indicate an upper respiratory focus, and sputum may be difficult to obtain from elderly residents, reducing its utility here. Option D, " Legionella serology, " is specific for diagnosing Legionella pneumophila, which causes Legionnaires’ disease, typically presenting with fever, cough, and sometimes gastrointestinal symptoms, often in association with water sources. While possible, the lack of mention of pneumonia or water exposure, combined with the upper respiratory symptoms, makes Legionella serology less likely as the best initial test. Serology also requires time for antibody development, delaying diagnosis compared to direct sampling.
The CBIC Practice Analysis (2022) and CDC guidelines for outbreak management in long-term care facilities (e.g., " Prevention Strategies for Seasonal Influenza in Healthcare Settings, " 2018) prioritize rapid respiratory pathogen identification, with nasopharyngeal swabs being the preferred method for viral detection. Given the symptom profile and outbreak context, Option C is the most effective and immediate diagnostic tool to determine the causative agent.
Which of the following pathogens is associated with the highest risk of seroconversion after percutaneous exposure?
Options:
Shigella
Syphilis
Hepatitis A
Hepatitis C
Answer:
DExplanation:
Among the listed pathogens, Hepatitis C has the highest risk of seroconversion following a percutaneous exposure, though it ' s important to note that Hepatitis B actually has the highest overall risk. However, since Hepatitis B is not listed among the options, the correct choice from the available ones is Hepatitis C.
The APIC Text confirms:
“The average risk of seroconversion after a percutaneous injury involving blood infected with hepatitis C virus is approximately 1.8 percent”.
The other options are not bloodborne pathogens typically associated with high seroconversion risks after needlestick or percutaneous exposure:
A. Shigella – transmitted fecal-orally, not percutaneously.
B. Syphilis – transmitted sexually or via mucous membranes.
C. Hepatitis A – primarily fecal-oral transmission, low occupational seroconversion risk.
Which of the following options describes a correct use of personal protective equipment?
Options:
Personal eyeglasses should be worn during suctioning.
Surgical masks should be worn during lumbar puncture procedures.
Gloves should be worn when handling or touching a cardiac monitor that has been disinfected.
Eye protection should be worn when providing patient care it at risk of spreading respiratory disease after unprotected exposure.
Answer:
BExplanation:
According to CDC and APIC guidelines, a surgical mask is required when performing lumbar punctures to prevent bacterial contamination (e.g., meningitis caused by droplet transmission of oral flora).
Why the Other Options Are Incorrect?
A. Personal eyeglasses should be worn during suctioning – Incorrect because eyeglasses do not provide adequate eye protection. Goggles or face shields should be used.
C. Gloves should be worn when handling or touching a cardiac monitor that has been disinfected – Not necessary unless recontamination is suspected.
D. Eye protection should be worn when providing patient care after unprotected exposure – Eye protection should be used before exposure, not just after.
CBIC Infection Control Reference
APIC states that surgical masks must be worn for procedures such as lumbar puncture to reduce infection risk.
An infection preventionist (IP) is reviewing blood cultures and notices several results with Arcanobacterium, coagulase-negative Staphylococcus, and Corynebacterium. What action is needed from the IP?
Options:
Disregard the results.
Call the Medical Staff Officer and declare there is an outbreak.
Work up each case as a healthcare-acquired bloodstream infection.
Collaborate with the lab manager to determine if there are trends or changes in practice.
Answer:
DExplanation:
The CBIC Certified Infection Control Exam Study Guide (6th edition) emphasizes that certain organisms commonly recovered from blood cultures—such as Arcanobacterium, coagulase-negative Staphylococcus, and Corynebacterium—are frequently associated with skin contamination rather than true bloodstream infection. When multiple blood cultures yield these organisms, the infection preventionist must assess whether the findings represent contamination related to collection practices rather than immediately assuming infection or outbreak.
The most appropriate action is to collaborate with the laboratory manager and clinical teams to evaluate potential trends, specimen collection techniques, and changes in practice. This includes reviewing blood culture contamination rates, assessing skin antisepsis procedures, evaluating staff competency, and determining whether there has been an increase associated with a specific unit, shift, or collection method. Surveillance data and laboratory quality indicators are essential tools in this evaluation.
Option A is incorrect because results should never be disregarded without assessment. Option B is premature, as the organisms listed are not typical outbreak pathogens and require further analysis before escalation. Option C is inappropriate because these organisms do not automatically meet criteria for healthcare-associated bloodstream infection without supporting clinical evidence.
This scenario reflects a core CIC® exam concept: infection preventionists must apply epidemiologic principles, collaborate with laboratory services, and use data-driven analysis to differentiate contamination from infection and to guide quality improvement efforts.
=========
The MOST common reason for contamination of compounded pharmaceutical products is:
Options:
Direct touch by personnel
Inadequate laminar airflow
Infrequent environmental sampling
Inappropriate storage of pharmaceutical items
Answer:
AExplanation:
The CBIC Certified Infection Control Exam Study Guide (6th edition) identifies direct touch contamination by personnel as the most common cause of contamination of compounded pharmaceutical products. Human contact—particularly hands, gloves, sleeves, or improper manipulation of sterile components—is the greatest source of microbial contamination during compounding activities.
Even when engineering controls such as laminar airflow workbenches and cleanrooms are functioning correctly, contamination can occur if aseptic technique is not strictly followed. Touching sterile vial stoppers, syringe tips, needle hubs, or critical sites with nonsterile hands or gloves introduces microorganisms directly into the product. The Study Guide emphasizes that aseptic technique, hand hygiene, glove use, and competency validation are essential to preventing contamination.
Option B, inadequate laminar airflow, can contribute to contamination but is less common than direct touch errors and is usually detected through certification and monitoring. Option C, infrequent environmental sampling, does not cause contamination but may delay detection of problems. Option D, inappropriate storage, can affect product stability but is not the primary cause of contamination during compounding.
For CIC® exam preparation, it is critical to recognize that human factors are the leading source of contamination in sterile compounding. Infection prevention strategies therefore focus heavily on staff training, competency assessment, observation, and adherence to aseptic technique standards to reduce contamination risk.
Documentation of each steam sterilization cycle should include which of the following pieces of information?
Options:
Load contents
Machine model number
Date sterilizer was cleaned
Initials of the person who prepared the instrument set
Answer:
AExplanation:
Documentation of each steam sterilization cycle is a regulatory and quality requirement. It must include load contents, the sterilizer ID, date, cycle number, and the person who assembled the load. These details support traceability and quality assurance.
The APIC Text states:
“Each item or package should be labeled with a lot-control identifier that includes the sterilizer identification number or code, a detailed list of the contents, an identifier for the person who assembled the package, the date of sterilization, the cycle number...”
Other options like the machine model number or date sterilizer was cleaned are not routine documentation elements for every cycle.
An infection preventionist is educating healthcare personnel on standard precautions and isolation requirements. Sessions consist of large group lectures and demonstrations. Three months later, a carbapenem-resistant Enterobacterales (CRE) outbreak occurs. Which of the following strategies will minimize the risk of a subsequent outbreak?
Options:
Reviewing the educational content to ensure that it includes the most recent recommendations
Creating a test to be used at the end of the education sessions to evaluate learning
Recording the lecture to allow staff more time to review the recording when convenient
Meeting with the managers to assess staff compliance with isolation precautions
Answer:
DExplanation:
The Certification Study Guide (6th edition) stresses that education alone is insufficient to ensure sustained adherence to infection prevention practices. While lectures and demonstrations are valuable for knowledge dissemination, they do not guarantee consistent behavioral compliance over time. In this scenario, the occurrence of a CRE outbreak three months after education indicates a gap between knowledge and practice.
To minimize the risk of a subsequent outbreak, the most effective strategy is directly assessing staff compliance with isolation precautions, which is best accomplished by engaging managers and leadership. The study guide emphasizes the importance of monitoring, auditing, and feedback as core components of an effective infection prevention program. Managers are uniquely positioned to observe daily practice, reinforce expectations, and hold staff accountable for adherence to standard and transmission-based precautions.
The other options focus primarily on educational reinforcement rather than practice validation. Updating content, testing knowledge, or offering recorded lectures may improve awareness but do not address whether staff are actually implementing precautions correctly at the point of care. CRE transmission is most often linked to failures in hand hygiene, contact precautions, and environmental cleaning—issues that require ongoing observation and performance management, not passive education.
This question reflects a common CIC exam theme: preventing outbreaks requires behavioral verification and leadership engagement, not education alone. By assessing and reinforcing compliance through managers, the infection preventionist addresses the root cause of transmission risk and supports sustainable prevention.
A laboratory has received specimens labeled eye drainage for four patients. In preparing an action plan, the infection preventionist should do which of the following FIRST?
Options:
Cohort the patients based on the presence of eye drainage.
Monitor hand-washing practices of staff and visitors.
Determine the location of the patients.
Conduct pulsed-field gel electrophoresis.
Answer:
CExplanation:
The CBIC Certified Infection Control Exam Study Guide (6th edition) emphasizes that when a potential cluster of infections is identified, the first priority is situational awareness. Before implementing control measures or advanced laboratory analysis, the infection preventionist must determine whether the cases are epidemiologically linked. Identifying the location of the patients—such as whether they are on the same unit, service, or clinic—is the essential first step in assessing the likelihood of transmission or a common source.
Option C is correct because determining patient location allows the IP to evaluate spatial and temporal relationships, which form the foundation of outbreak investigation. If the patients are colocated, this may indicate shared staff, equipment, or environmental exposure, guiding immediate and targeted interventions.
Cohorting patients (Option A) is premature without confirming proximity or transmission risk. Monitoring hand hygiene (Option B) is an important control measure but should follow confirmation of potential spread or shared risk factors. Pulsed-field gel electrophoresis (Option D) is an advanced molecular typing method and is never an initial step; it is reserved for later stages when epidemiologic evidence suggests related cases.
For the CIC® exam, this question tests understanding of outbreak investigation sequencing. The Study Guide consistently reinforces that defining who, where, and when comes before interventions or laboratory typing, making determination of patient location the correct first action.
A 21-ycnr-old college student was admitted with a high fever. The Emergency Department physician be gan immediate treatment with intravenous vancomycin and ceftriaxone while awaiting blood, urine, and cerebrospinal fluid cultures. The following day. the cultures of both the blood and the cerebrospinal fluid were reported to be growing meningococci. The patient was placed on precautions on admission. Which of the following is correct?
Options:
Droplet precautions may be discontinued after 24 hours of therapy.
Droplet precautions must continue
Airborne precautions may be discontinued after 24 hours of therapy.
Airborne precautions must continue.
Answer:
AExplanation:
Meningococcal infections, such as Neisseria meningitidis, are transmitted via respiratory droplets. According to APIC and CDC guidelines, patients with meningococcal disease should be placed on Droplet Precautions upon admission. These precautions can be discontinued after 24 hours of effective antibiotic therapy.
Why the Other Options Are Incorrect?
B. Droplet precautions must continue – Droplet Precautions are not needed beyond 24 hours of appropriate therapy because treatment rapidly reduces infectiousness.
C. Airborne precautions may be discontinued after 24 hours of therapy – Meningococcal infection is not airborne, so Airborne Precautions are never required.
D. Airborne precautions must continue – Incorrect because meningococci do not transmit via airborne particles.
CBIC Infection Control Reference
According to APIC guidelines, Droplet Precautions should be maintained for at least 24 hours after effective antibiotic therapy initiation.
The operating room director asks the infection preventionist (IP) to join a team focusing on the purchase of robotic surgical equipment. What item will the IP review FIRST?
Options:
Cost of the equipment
Effect of equipment on length of surgery
Storage of the equipment between surgical cases
Manufacturer’s instructions for use
Answer:
DExplanation:
The CBIC Certified Infection Control Exam Study Guide (6th edition) emphasizes that when evaluating new medical or surgical equipment, the first priority for the infection preventionist is reviewing the manufacturer’s instructions for use (IFU). The IFU provides critical information regarding cleaning, disinfection, sterilization, handling, storage, and maintenance requirements, all of which directly impact infection prevention and patient safety.
Robotic surgical equipment often includes complex components, lumens, joints, and reusable instruments that may require specialized reprocessing methods. The IP must ensure that the facility has the infrastructure, staffing, competency, and resources to meet the IFU requirements before purchase. Failure to comply with manufacturer instructions places the organization at risk for ineffective reprocessing, device contamination, healthcare-associated infections, and regulatory noncompliance.
The other options are secondary considerations. Cost (Option A) and operative time impact efficiency and budgeting but do not address infection risk. Storage between cases (Option C) is important but cannot be properly evaluated without first understanding IFU requirements. Length of surgery (Option B) may influence infection risk but is not within the primary evaluative scope of infection prevention during equipment selection.
For the CIC® exam, it is essential to recognize that IFU review is the foundational step in product evaluation. Infection preventionists must confirm that equipment can be safely and consistently reprocessed according to manufacturer specifications before any operational or financial considerations are addressed.
==========
The infection preventionist understands that the heating, ventilation and air conditioning (HVAC) systems in the facility can be a risk factor for healthcare-acquired infections. What is the MOST likely risk from the HVAC system for patients in a Pediatric Oncology unit?
Options:
Methicillin-resistant Staphylococcus aureus (MRSA)
Norovirus
Aspergillus spp.
Clostridioides difficile
Answer:
CExplanation:
Patients in pediatric oncology units are highly immunocompromised, making them particularly susceptible to opportunistic fungal infections such as Aspergillus spp. HVAC systems, especially if improperly maintained or contaminated, can disseminate fungal spores into patient care areas.
According to the APIC Text (Chapter 116 – HVAC Systems), fungal spores such as Aspergillus can be transmitted via HVAC systems. These infections have been linked to contaminated air ducts, faulty air filters, and construction-related air disturbances. Outbreaks of aspergillosis are frequently associated with construction near patient care areas and are particularly dangerous for immunocompromised patients, including pediatric oncology patients.
Additional data from APIC Text (Chapter 45 – Infection Prevention in Oncology Patients) reinforces that Aspergillus spp. infections in oncology and immunocompromised patients are primarily airborne and are most often disseminated via HVAC systems.
Incorrect answer rationale:
A. MRSA – Typically spread via direct contact, not HVAC.
B. Norovirus – Spread via fecal-oral route and contaminated surfaces, not airborne HVAC.
D. Clostridioides difficile – Spread via contact with spores on surfaces, not through the air.
Which of the following patients with human immunodeficiency virus infection requires Airborne precautions?
Options:
24-year-old male newly diagnosed with a CD4 count of 70
28-year-old female with Mycobacterium avium in sputum
36-year-old male with cryptococcal meningitis
46-year-old female with a cavitary lesion in upper lobe
Answer:
DExplanation:
HIV patients require Airborne Precautions if they have tuberculosis (TB). A cavitary lesion in the upper lobe is highly suggestive of active pulmonary TB, which requires Airborne Precautions due to aerosolized transmission.
Why the Other Options Are Incorrect?
A. 24-year-old male newly diagnosed with a CD4 count of 70 – Low CD4 count alone does not warrant Airborne Precautions unless there is active TB or another airborne pathogen.
B. 28-year-old female with Mycobacterium avium in sputum – Mycobacterium avium complex (MAC) is not airborne, and standard precautions are sufficient.
C. 36-year-old male with cryptococcal meningitis – Cryptococcus neoformans is not transmitted via the airborne route, so Airborne Precautions are unnecessary.
CBIC Infection Control Reference
Patients with HIV and suspected TB require Airborne Precautions until TB is ruled out.
A healthcare personnel has an acute group A streptococcal throat infection. What is the earliest recommended time that this person may return to work after receiving appropriate antibiotic therapy?
Options:
8 hours
24 hours
48 hours
72 hours
Answer:
BExplanation:
The correct answer is B, " 24 hours, " as this is the earliest recommended time that a healthcare personnel with an acute group A streptococcal throat infection may return to work after receiving appropriate antibiotic therapy. According to the Certification Board of Infection Control and Epidemiology (CBIC) guidelines, which align with recommendations from the Centers for Disease Control and Prevention (CDC), healthcare workers with group A Streptococcus (GAS) infections, such as streptococcal pharyngitis, should be treated with antibiotics (e.g., penicillin or a suitable alternative) to eradicate the infection and reduce transmission risk. The CDC and Occupational Safety and Health Administration (OSHA) guidelines specify that healthcare personnel can return to work after at least 24 hours of effective antibiotic therapy, provided they are afebrile and symptoms are improving, as this period is sufficient to significantly reduce the bacterial load and contagiousness (CBIC Practice Analysis, 2022, Domain III: Infection Prevention and Control, Competency 3.2 - Implement measures to prevent transmission of infectious agents).
Option A (8 hours) is too short a duration to ensure the infection is adequately controlled and the individual is no longer contagious. Option C (48 hours) and Option D (72 hours) are longer periods that may apply in some cases (e.g., if symptoms persist or in outbreak settings), but they exceed the minimum recommended time based on current evidence. The 24-hour threshold is supported by studies showing that GAS shedding decreases substantially within this timeframe with appropriate antibiotic treatment, minimizing the risk to patients and colleagues (CDC Guidelines for Infection Control in Healthcare Personnel, 2019).
The infection preventionist’s role includes enforcing return-to-work policies to prevent healthcare-associated infections (HAIs), aligning with CBIC’s emphasis on timely and evidence-based interventions to control infectious disease transmission in healthcare settings (CBIC Practice Analysis, 2022, Domain III: Infection Prevention and Control, Competency 3.1 - Collaborate with organizational leaders). Compliance with this recommendation also supports occupational health protocols to balance staff safety and patient care.
Microfiber cloths and mops are preferred over cotton because microfiber:
Options:
Is more cost effective.
Is positively charged to better attract dirt.
Can be laundered and dried with other textiles.
Is versatile for both smooth and rough surfaces.
Answer:
BExplanation:
The CBIC Certified Infection Control Exam Study Guide (6th edition) explains that microfiber cleaning materials are preferred over traditional cotton cloths and mops because of their electrostatic properties, which enhance cleaning effectiveness. Microfiber is composed of very fine synthetic fibers that become positively charged, allowing them to attract and trap negatively charged dirt, dust, and microorganisms rather than simply pushing them across surfaces.
This electrostatic attraction enables microfiber to remove a significantly higher percentage of bacteria and organic material from surfaces compared to cotton, even when used with less cleaning solution or disinfectant. The split fiber structure also increases surface area, allowing microorganisms and debris to be captured within the fibers rather than redistributed. These properties make microfiber particularly effective for environmental cleaning in healthcare settings, where surface contamination contributes to transmission of healthcare-associated infections.
Option A is incorrect because microfiber products are often more expensive initially, though they may be cost-effective over time. Option C is incorrect because microfiber must be laundered separately under specific conditions to maintain effectiveness. Option D may be true but is not the primary reason for preference.
For the CIC® exam, it is important to recognize that microfiber’s positive charge and superior ability to attract and retain microorganisms are the key reasons it is favored over cotton for environmental cleaning and infection prevention.
An 84-year-old male with a gangrenous foot is admitted to the hospital from an extended-care facility (ECF). The ECF is notified that the wound grew Enterococcus faecium with the following antibiotic sensitivity results:
ampicillin – R
vancomycin – R
penicillin – R
linezolid – S
This is the fourth Enterococcus species cultured from residents within the same ECF wing in the past month. The other cultures were from two urine specimens and a draining wound. The Infection Preventionist (IP) should immediately:
Options:
Notify the medical director of the outbreak.
Compare the four culture reports and sensitivity patterns.
Conduct surveillance cultures for this organism in all residents.
Notify the nursing administrator to close the wing to new admissions.
Answer:
AExplanation:
The scenario describes a potential outbreak of multidrug-resistant Enterococcus faecium in an extended-care facility (ECF) wing, indicated by four positive cultures (including the current case and three prior cases from urine and a draining wound) within a month. The organism exhibits resistance to ampicillin, vancomycin, and penicillin, but sensitivity to linezolid, suggesting a possible vancomycin-resistant Enterococcus (VRE) strain, which is a significant concern in healthcare settings. The Certification Board of Infection Control and Epidemiology (CBIC) emphasizes the importance of rapid outbreak detection and response in the " Surveillance and Epidemiologic Investigation " domain, aligning with Centers for Disease Control and Prevention (CDC) guidelines for managing multidrug-resistant organisms (MDROs).
Option A, " Notify the medical director of the outbreak, " is the most immediate and critical action. Identifying an outbreak—defined by the CDC as two or more cases of a similar illness linked by time and place—requires prompt notification to the facility’s leadership (e.g., medical director) to initiate a coordinated response. The presence of four Enterococcus cases, including a multidrug-resistant strain, within a single ECF wing over a month suggests a potential cluster, necessitating urgent action to assess the scope, implement control measures, and allocate resources. The CDC’s " Management of Multidrug-Resistant Organisms in Healthcare Settings " (2006) recommends immediate reporting to facility leadership as the first step to activate an outbreak investigation team, making this the priority.
Option B, " Compare the four culture reports and sensitivity patterns, " is an important subsequent step in outbreak investigation. Analyzing the antibiotic susceptibility profiles and culture sources can confirm whether the cases are epidemiologically linked (e.g., clonal spread of VRE) and guide treatment and control strategies. However, this is a detailed analysis that follows initial notification and should not delay alerting the medical director. Option C, " Conduct surveillance cultures for this organism in all residents, " is a proactive measure to determine the prevalence of Enterococcus faecium, especially VRE, within the wing. The CDC recommends targeted surveillance during outbreaks, but this requires prior authorization and planning by the outbreak team, making it a secondary action after notification. Option D, " Notify the nursing administrator to close the wing to new admissions, " may be a control measure to prevent further spread, as suggested by the CDC for MDRO outbreaks. However, closing a unit is a significant decision that should be guided by the medical director and infection control team after assessing the situation, not an immediate independent action by the IP.
The CBIC Practice Analysis (2022) and CDC guidelines prioritize rapid communication with leadership to initiate a structured outbreak response, including resource allocation and policy adjustments. Given the multidrug-resistant nature and cluster pattern, notifying the medical director (Option A) is the most immediate and appropriate action to ensure a comprehensive response.
A hospital wants to launch an alternative care site due to an influx of patients from a mass casualty incident. An infection preventionist should be engaged to BEST determine:
Options:
Optimal medical care being offered.
Staffing of licensed and unlicensed staff.
Measures to keep all individuals healthy.
Requirements for providing direct patient care.
Answer:
DExplanation:
The Certification Study Guide (6th edition) outlines the critical role of the infection preventionist (IP) in emergency preparedness and response, particularly when healthcare systems activate alternate or alternative care sites during mass casualty incidents or public health emergencies. In these situations, the IP’s primary responsibility is to determine the infection prevention and control requirements necessary to safely provide direct patient care in nontraditional settings.
Alternate care sites often lack the infrastructure of acute care hospitals, such as standard ventilation, hand hygiene facilities, isolation rooms, or routine environmental services. The study guide emphasizes that infection preventionists must assess risks related to patient placement, cohorting, isolation precautions, environmental cleaning, waste management, water safety, and availability of personal protective equipment. These determinations directly influence whether patient care can be delivered safely and sustainably under emergency conditions.
The other options fall outside the IP’s primary scope. Decisions about optimal medical care and staffing models are led by clinical and administrative leadership. “Measures to keep all individuals healthy” is overly broad and does not reflect the IP’s focused, operational role during emergency site activation.
CIC exam questions frequently test understanding of role delineation during emergency management. The infection preventionist’s expertise is best applied to defining infection control standards and requirements that enable safe direct patient care—making option D the most accurate and appropriate answer.
The infection preventionist (IP) is reviewing a laboratory report that indicates the presence of Enterococcus faecium in a 76-year-old patient’s urine culture. The patient has no symptoms of a urinary tract infection. The IP’s accurate interpretation of this result is that the patient:
Options:
Should be placed in isolation due to the risk of airborne transmission.
Has an active infection and requires immediate treatment with antibiotics.
Is colonized with the bacteria and does not require treatment at this time.
Has a pseudo-infection, which could be caused by contamination of the sample.
Answer:
CExplanation:
The CBIC Certified Infection Control Exam Study Guide (6th edition) emphasizes the importance of distinguishing colonization from infection when interpreting microbiology results. Colonization refers to the presence of microorganisms on or within the body without causing clinical signs or symptoms of disease. In older adults, especially those in healthcare settings, asymptomatic bacteriuria is common and does not meet criteria for a urinary tract infection (UTI).
In this scenario, the presence of Enterococcus faecium in a urine culture in the absence of urinary symptoms—such as dysuria, urgency, fever, or suprapubic pain—indicates colonization rather than infection. The Study Guide notes that treating asymptomatic bacteriuria does not improve patient outcomes and may contribute to antimicrobial resistance, adverse drug events, and unnecessary healthcare costs. Therefore, antibiotics are not indicated.
Option A is incorrect because Enterococcus species are not transmitted via the airborne route; Standard Precautions are sufficient. Option B is incorrect because laboratory findings alone do not define infection without corresponding clinical symptoms. Option D is less accurate because contamination is more likely with mixed flora or improper collection; isolation of a known urinary colonizer in an asymptomatic patient is more consistent with colonization.
Accurate interpretation of such findings supports antimicrobial stewardship principles and aligns with evidence-based infection prevention practices tested on the CIC® exam.
==========


